Introduction
Advances in modern medicine have created methods of artificial respiration, resuscitation, as well as a plethora of techniques and technologies which have enabled doctors to prolong the life of patients well beyond the capacities of failing organs or a distinct inability to properly care for oneself as seen in the case of coma patients. Yet, despite such advances, it is at times questioned whether prolonging the life of a patient who is obviously going to die soon (seen in cases involving centenarians), those are brain dead yet physically alive (noted in instances where patients have been affected by severe strokes), or those who are beyond recovery yet are being kept alive through the aid of machines (i.e. those involved in severe accidents) is a practical or ethical recourse since not only is it cost prohibitive but it denies such individuals the right to a “natural death” so to speak. The Hippocratic oath of physicians in such instances compels doctors to care and prolong the life of the patient as need be, however, this brings up an ethical conundrum wherein by prolonging the life of a patient beyond the means from which they could make a full or partial recovery, such as in instances where they would be unable to move, talk, speak or interact with the outside world, would this not be considered an unethical action since it denies a person the right to a clean death without having to endure undue hardship that could have been avoided. Various studies further reinforce the debate on an individual’s innate right to a clean death by showing that individuals who are in commas or considered brain dead actually have some form of awareness yet are unable to function in the normal sense. This leaves them trapped in a state of perpetual confinement which in itself can be considered a form of torture. In such instances where no medical procedure can be done which could resolve the situation it is often considered more merciful to simply allow them to die. Other cases along this same train of thought involve terminal cancer patients who are experiencing extreme pain. It is at times thought to be more ethical to allow them the mercy of painless death rather than prolong their agony through the use of modern medical procedures. Another factor that should be taken into consideration is the cost prohibitiveness of prolonging life in cases where it is neither practical nor reasonable. Medical procedures and devices meant to prolong the life of a patient in terminal condition are by no means inexpensive and can financially cripple a large percentage of families. When taking such a factor and combining it with a situation involving a patient that has no chance for recovery after experiencing severe physical trauma, this shows that in terms of financial practicality resuscitating a person that cannot effectively function no matter what can be done is the height of folly. It must also be noted that patients who are aware of the financial burden of their situation often experience extreme anxiety and depression which creates a significant degree of emotional stress. After taking all the factors mentioned into consideration, it is often the case that people would wish to avoid a fate of extreme pain, being unable to move and talk or becoming a significant financial burden to their family, this is where the concept of DNR (Do Not Resuscitate) comes in to play.
Hypothesis
It is the hypothesis of this study that despite the ethical arguments against DNR, the fact that it enables an individual to have a natural death and frees them from their discomfort and pain makes it an acceptable medical practice based on its positive effects,
Do Not Resuscitate
Introduction
A DNR (Do Not Resuscitate) is defined as legal order that embodies the wish of the client not be subjected to CPR or types of advanced cardiac life support if their heartbeat or breathing were to stop. From a legal perspective a DNR is the embodiment of an individual’s desire to die a “natural death” without their life being prolonged in an artificial manner. When a DNR is issued by the hospital and implemented by the state it is usually the case that the order has already taken into consideration the quality of life of the patient, the seriousness of their current condition and the fact that due to the inherent limitation of modern medicine nothing can truly be done to resolve such an issue. This section delves into the concept of DNR and attempts to explain what is it for, what complications may arise and what are ethical decisions behind its implementation.
Indications for do not resuscitate
Indicators applicable to DNR vary due to a wide assortment of cases and situations; however, one generally accepted rule of thumb is that a DNR is usually applied to terminally ill patients. This can consist of individuals suffering from advanced stages of various forms of cancer, those who have reached a considerable age (85 and above), individuals suffering from injuries that cannot be remedied by modern medicine and a variety of other cases where medical practices and technologies have reached their limit. Another indicator utilized for DNR orders are evaluations of a patient’s quality of life which can constitute their level of discomfort as a result of extreme amounts of pain (as seen in cases involving the elderly or those suffering from cancer), aspects related to whether or not they are able to function normally (seen in cases involving patients in comas) or have no hope of recovery despite being physically fine (normally attributed to individuals who are brain dead as a result of affixation or other similar types of actions that limit the supply of oxygen to the brain). Bacchetta et al. (2006)does state though that methods of evaluation differ based on factors related to the sociological acceptance of DNR within a particular country, the degree of religious influences that influence public opinion as well as the rules of the state where the medical institutions are present (Bacchetta et al., 2006:995-1000). Due to the sheer variety of social circumstances, state laws and religious influences, this creates a situation where an all encompassing standard medical practice involving DNR is not present. In fact, due to certain unique circumstances involving religious institutions and their interference in the rules an regulation of the local medical industry, DNRs are sometimes not present at all or are never offered to either the patient or his/her family members as seen in the case of Jordan.
Complications for do not resuscitate
First uttered by Allen Greenspan On December 6, 1996, the concept of irrational exuberance is one of the main proponents that influences the current negative societal concept related to DNR. This particular concept is based on the notion that people tend to base their behavior on the actions of other people resulting in unduly escalated values for particular concepts, ideas and methods of thinking regardless of their inherent justifiability. This can be seen in the case of the largely negative image attributed to DNR by the general public wherein it is viewed as an unethical aspect of modern day medicine. Do Yeun et al (2007) gives a more in-depth explanation of the current negative view against DNR by explaining that irrational exuberance has gripped the general public wherein their lack of knowledge regarding the processes involving DNR has led to various assumptions most of which are mere hearsay and conjecture (Do Yeun et al., 2007: 1153-1158). Such views have been further unduly influenced by various human rights groups who have been generalizing the right to life (as seen in the arguments presented regarding abortions) to the concept of DNR and have in effect created a generalized all encompassing social idea involving the supposedly unethical action of denying an individual the right to life despite their current quality of life. While such notions do have a certain ethical basis, they neglect to delve sufficiently into the concept of an individual’s right to a humane death and focus almost exclusively on the concept of life. This particular type of one-sided “blind” argument has unfortunately sufficiently ensconced itself into the present day societal consciousness that is has in effect adversely affected the implementation of DNR. Some of the manifestations of negative outlook on DNR come in the form of hospitals being reluctant to even bring up a DNR order due to the possible backlash that may occur such as those originating from the family of the patient or a variety of advocacy groups. In the end, the ones that are most adversely affected by this are the patients themselves who will have to endure a painful and uncomfortable prolonged artificial life with the only ray of light being that the next time they have a seizure they would hopefully die.
Do Not Resuscitate Orders
Introduction (what do CPR and DNR orders mean?)
CPR orders consist of instances where a patient is to be resuscitated should they enter into a form of cardiac arrest or if their breathing were to stop for some apparent reason. DNR orders on the hand prevent the implementation of CPR orders as a form of directive that embodies the wish of the client to die a natural death without having to endure the pain and discomfort that comes with an artificially prolonged existence. This section will explore the various as to when CPR can be applied, when it can be withheld and its current relationship with DNR orders.
When should CPR be administered?
CPR is usually administered in cases where paramedics are attempting to preserve an individual’s brain functions through the restoration of blood flow and breathing in a person that has recently gone into cardiac arrest. It is a method of resuscitation utilized in order to ensure that a person’s blood flow can be restored to a point that the brain and other parts of the body are not deprived of oxygen which preserves the overall ability of that individual to continue to function. One point of confusion that should be addressed at this particular point is that CPR is a method of resuscitation and not revival, it is often the case that both terminologies and the idea behind them is often interchanged by the uninitiated, however, what must be understood is that CPR is only applicable in cases where there is a chance that a patient can still be resuscitated given certain parameters such as their current condition, the point of time between when they lost a pulse and the moment where resuscitation has started as well as a variety of other factors. The concept of revival on the other hand is applicable to cases where the individual is past the point of resuscitation and has been declared deceased. It is from this that CPR should not be considered a “cure all” so to speak, but rather is a highly specific medical practice that is applicable only to a certain number of cases where a patient can actually be successfully resuscitated.
When can CPR be withheld?
Before moving forward it must be noted that CPR should never be construed as being 100% effective as seen on television shows and in movies. In fact, even in tightly controlled clinical situations CPR can be ineffective given several circumstances such as the physical condition of the patient, the progression of a particular type of disease and even their age.
The following is the popular culture view on CPR:
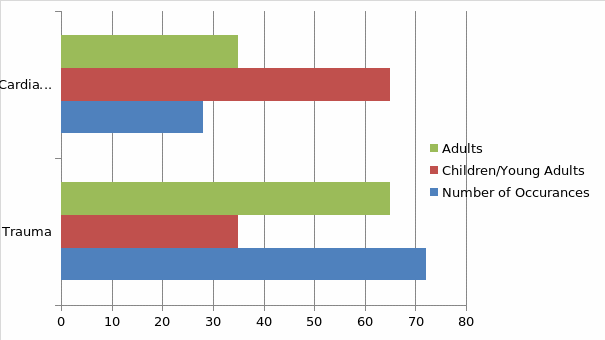
It shows how in most modern day TV shows most patients who need CPR either suffer from cardiac arrest or severe trauma with only 28 percent of cases being a result of cardiac arrest while 72 percent was due to trauma. Furthermore various televisions programs portray 65% of children/young adults as suffering from cardiac arrests while conversely 65% of adults suffer from significant trauma, both of which necessitate circumstances where CPR is warranted.
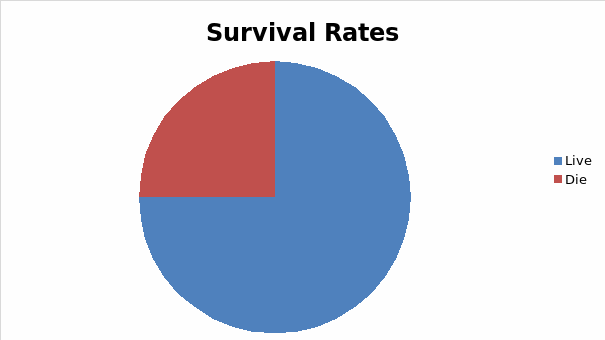
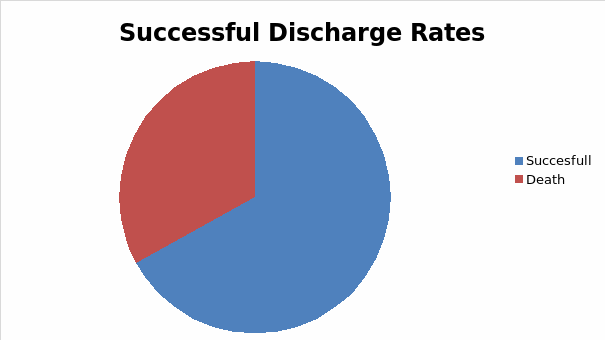
From the following graphs it can be seen that the popular culture view on survival rates after cardiac arrest (especially in cases involving children and young adults) is highly optimistic with 75% of cases surviving the immediate effects of CPR and 67% making a full recovery and successful being discharged from the hospital. In reality, studies such as a Meta analysis which examined 20,000 cases of patients that have had CPR show the following data:
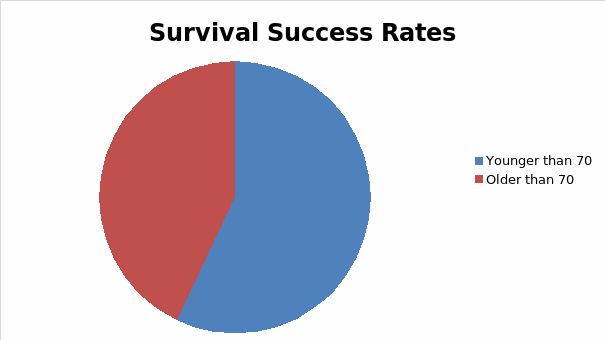
The results of the analysis involving real world data shows that on average only 16.2 CPR cases involving people younger than 70 were successful, while those that were older than 70 had a success rate of 12.2. What this reveals is that CPR success rates are not what they appear to be and that the general perception surrounding the process and its success rates has been highly exaggerated by popular culture movies and TV shows. Based on the Meta analysis it was seen that 72.9 percent of cases involving patients who received CPR within hospital settings died within 72 hours due to a variety of complications with 1.6 percent of individuals that were successfully resuscitated experiencing varying degrees of permanent neurological impairment. This is in stark contrast to the recovery and discharge rates assumed by popular culture programming and is evidence of the disparity between the assumptions of nonmedical personnel regarding the processes that involve CPR. It is based on this that when examining issues involving when CPR can be withheld it must be done from the perspective of relevant medical data and the perspective of the attending physician.
CPR is usually withheld in instances where it has been determined that a patient is beyond the point of effective resuscitation or in cases where it has been determined that even if resuscitation were possible the patient would have already received considerable brain damage as result of oxygen deprivation and would result in them becoming what is commonly known as a “vegetable”. Gouda, Al-Jabbary, & Fong (2010) elaborates on the ethics of such a concept by explaining that most medical practitioners practice medicine for the benefit of their patients (Gouda, Al-Jabbary, & Fong, 2010:2149-2153). As such, they attempt to avoid practices which are deemed detrimental to the well being of such an individual. EMTs in their capacity as emergency workers often come across such instances of “detrimental resuscitation” in instances where a victim has been denied oxygen for an extended period of time. It is generally understood that CPR should only be implemented in situations where it is feasible that the individual in question can make a recovery. Other instances where CPR can be withheld is if the patient has a standing DNR order in place that is known by the hospital. If the DNR order is legitimate and enforced by the state CPR cannot be administered since it is the patient’s wish to die a natural death rather than prolong his/her life artificially.
When is CPR “futile”?
CPR can be construed as being futile in cases where a patient is “beyond help” as defined by the standard methods of medical evaluation. This can consist of a variety of circumstances such as the brain being denied oxygen for an extended period of time, an individual’s injuries being far too severe or in instances where despite resuscitation it is likely that a relapse will occur within the immediate future. One of the more notable examples of futile CPR can be seen in the case of hurricane Katrina where emergency medical services encountered dozens of victims of the flood yet did not perform any measure of resuscitation due to length of time spent underwater. Another example is presented by Hite (2000) involving a patient who was suffering from lung cancer resulting from excessive smoking (Hite, 2000: 307). The patient had been revived multiple times by the nurses on duty due to his failing health, however, due to the severity of his condition coupled with the fact that there was no means by which a donor could be found within the time frame needed the multiple times the patient was revived was inherently futile since there was no way an appropriate method of treatment could be implemented in time before his condition deteriorated to the point where resuscitation could no longer be performed. It is based on this that the concept of “futile CPR” is applicable to cases where despite resuscitation it is unlikely that process will result in any lasting benefit for the patient. The point of CPR is to revive an individual who still has a chance at life and to sustain it to the point that other processes can be implemented so as to ensure that a relapse will not occur. When it comes to futile cases of CPR, even if a patient is revived, there are no effective processes which can be implemented after revival to sufficiently ensure that a relapse will not occur. This is often seen in cases involving the elderly, those suffering from grievous physical injuries or instances involving a particularly harmful viral infection. It is when such instances present themselves that the family of the patient is often presented with a DNR option. What must be understood is that while CPR is a life saving measure, it also places a significant strain on the body especially in instances where defibrillation is utilized. Case evaluations examining individuals who have experienced multiple instances of CPR as a direct result of their present status often show various complications occurring to a patient’s medical condition resulting in either greater discomfort or a far less likely chance of recovery due to the significant amount of strain placed on the body. This is not to say that CPR is an adverse practice, rather, it is more accurate to say that there are instances where CPR is beneficial to a patient and others where it is futile and does nothing but prolong the discomfort of the patient due to the inherent limitation of modern medicine from sufficiently being able to address their current medical condition. Lyon et al. (2008) explains this best by stating that while it is the prerogative of doctors and various medical practitioners to do all that they can to improve the condition of a patient, there are instances where no amount of medicine, surgery or technique can be done to prevent an individual’s untimely demise (Lyon et al., 2008: 459-469). In such instances it is no longer a matter of ensuring that a patient survives, rather, it is more of a prerogative that their passing be made as peaceful as possible so as to give them the dignity of a humane death rather than prolong both their suffering and that of their loved ones. When taking such a view into consideration, it can be seen that there are instances where performing futile CPR can actually be considered more of a detriment rather than a benefit to a patient. This often involves cases where revival results in either undue hardship for the patient (ex: in instances where a patient is experiencing extreme pain due to his/her body being ravaged by cancer) without any positive benefit coming from the act of resuscitation since the patient cannot be helped by any current medical practices. As such, it is important to determine when CPR can be considered beneficial or not since this is often the basis behind the recommendation of a DNR order. The following section will thus elaborate on the concept and clarify what can be considered beneficial or detrimental CPR practices.
When is CPR not of benefit?
It is normally the case that CPR is considered a beneficial practice since it is a life saving measure meant to resuscitate an individual that has flat lined in order for other methods of care assistance to be implemented to ensure the continued survival of the patient. Yet, in cases where a patient’s quality of life is questioned it is at times questioned whether the act of CPR does not benefit the patient but rather prolongs that individual’s suffering. Such instances can be seen in cases where a patient is suffering from severe pain as a result of cancer, 3rd degree burns which cover more than 70% of their body, various types of grievous physical injury, a form of virulent disease and other such instances which can induce a significant amount of pain in an individual. Postovsky et al. (2004) elaborates on cases where CPR is not of benefit by explaining that while medical personnel are at times obligated by the very nature of their profession to implement various forms of resuscitation, of which CPR is included, it is often seen in such instances that the quality of life of the patient is not taken into consideration, rather, they are focused on the concept of saving and prolonging that individual’s life regardless of his/her current condition (Postovsky et al., 2004: 661-668). While it may be true that there are instances where CPR can be considered “futile” given the current status of the patient, this is not always the case wherein in some instances CPR can in fact restore a patient to a point that they can be further treated. Unfortunately, there are instances where resuscitation often leads to more pain, agony and discomfort for the patient since it restores them to a point of being able to live but does not alleviate the circumstances from which they are hospitalized. Various advocates of euthanasia such as Yuanmay et al. (2010) explain that it is often more humane and beneficial to allow a patient that has little to no hope of actual recovery to succumb to their condition and die without implementing CPR since this would at the very least end their suffering (Yuanmay et al., 2010: 445-455). Yuanmay et al. (2010) also proceeds to point out that the suffering and the quality of life of the patient often has negative side effects on the various family members present causing a variety of adverse psychological effects. Yuanmay et al. (2010) goes on to state that one of the inherent problems with current medical practices is that it focuses too much on the concepts of curing, resuscitation, and the prolonging of life that it neglects to take into account the quality of life of the patient and how keeping them alive can actually be construed as being similar to allowing the patient to continue to be tortured. Yuanmay et al. (2010) states that such opinions should not be misconstrued as being applicable to all cases but rather to a select few that involve patients with little to no hope of actual recovery. From this particular point of view it can be seen that CPR is not always a beneficial action and as such methods evaluating a patient’s quality of life should be taken into consideration prior to performing CPR.
How should the patient’s quality of life be considered?
Various individuals when they grow older develop various forms of disabilities and bodily deteriorations that entail certain medical requirements or observation in order to ensure that they don’t get worse. Teno et al. (2011) in his examination of the ethical considerations of caring for the elderly states that “in order to properly care for one’s parents this entails either having your parent’s move in with you in order to keep a closer eye on them or ensure that they receive proper medical treatment through the use of a retirement or medical care facility that specializes in caring for the elderly”
(Teno et al., 2011: 1040 -1047). What must be understood is that in certain cases involving highly sensitive individuals it becomes an almost daily necessity to ensure that they are doing well or rush them immediately to a proper care facility when complications occur. Since most individuals are busy with their own careers, personal lives and families it is often the case that proper medical care facilities or medical health requirements become necessary in any plan involving long term care health and support. While the quality of an individual’s life can be assessed in a myriad of different ways, in the context of CPR and DNR it is usually evaluated based on aspects related to pain management, the potential for the individual to recover as well as their ability to return to normalcy. Teno et al. (2011) assesses the quality of life of a patient by determining how well they will be able to function and utilizes a scale to indicate their overall quality of life. Those at the bottom consist of individuals who are comatose, cannot live without artificial methods of respiration and who suffer from advance forms of cancer where methods of pain relief are unable to mitigate a large percentage of their suffering. For Teno et al. (2011) such individuals should be given the option of a DNR or even euthanasia (though such a decision is controversial) given the extent of their suffering, their inability to live a normal life and the fact that there would be no method of actually helping them aside from artificially prolonging their existence which in itself is described by Teno et al. (2011) as a form of torture. The second category of the scale consists of individuals who have experienced grievous physical injury, have had numerous complications during their treatments or are “at risk” of potential death during surgery. Despite having such qualities Teno et al. (2011) explains that these individuals have a far better quality of life as compared to those at the bottom of the scale since, despite the various adverse characteristics that define such individuals, they at least have the “potential” to return to normalcy should the treatments, surgery and various methods of physical therapy prove to be effective. Lastly, those at the top of the scale are individuals who have very minor injuries, have no complications whatsoever and can be expected to return to their normal lives with little residual effects from their hospital stay. This group can be considered as having a high quality of life and is defined by Teno et al. (2011) as being the least likely to merit any form of DNR orders. From the point of view of Teno et al. (2011) DNR orders should only be offered or allowed to be put in place when patients fall under the lowest category of the Teno et al. (2011) scale. The reason behind this is due to the fact there can be no improvement in the quality of life in such cases, especially for those suffering from old age and advanced forms of cancer. It can only be expected to get worse over time with various methods of resuscitation only serving to prolong the “agony” of their continued existence. It is based on this that when it comes examining the quality of a patient’s life as the basis behind a DNR order, it must be assessed on the merits of potential improvement or progressive deterioration as seen in a case by case basis.
If CPR is deemed “futile”, should a DNR order be written?
In instances where CPR has been determined as “futile” by a licensed medical professional, a DNR order cannot necessarily be written due factors involving the informed consent of the patient/ family members or a health care power of attorney which explicitly indicates that a patient should not be revived. Berger (2003) elaborates on this by explaining that despite the inherent “futility” in attempting to revive someone that cannot be revived, medical professionals are still under the obligation to attempt resuscitation during such instances barring factors that are beyond medical care (i.e. arriving at a scene where the patient is clearly dead or beyond all hope of recovery such as being crushed, dismembered, etc.)
(Berger, 2003: 2270). Such actions are done regardless of any prior knowledge that the attempt would be useless and futile. The main reason behind this is due to an interpretation of the medical code of ethics which relates to patient care and resuscitation wherein medical personnel have to at least “try” to revive a patient despite the inherent futility. Accusations of medical malpractice and neglect from the family of the patient are also factors which are taken into consideration when it comes to CPR since it was noted in several cases involving “futile resuscitation” that family members reacted in an adverse manner towards hospital personnel and staff when presented with the notion that it would be futile to attempt any manner of resuscitation. Such cases often result in medical malpractice lawsuits which are costly and detrimental towards a hospital’s reputation, as such, it is usually the case that some attempts at resuscitation are implemented despite the fact that nothing can be done. Furthermore, it must be noted that the capacity of a doctor to create a DNR order is limited by the laws of the state, region, or country they are presently in. For example, in the case of the U.K. if a patient does not have the mental capability (i.e. is unconscious) the doctor is allowed to act in their best interest using “clinical judgment” as the basis behind issuing a DNR order. On the other hand, such a capacity is not inherent in the case of other countries such as the U.S., Japan, and various states within the Middle East. Differences in the capacity of doctors to utilize clinical judgment as the basis behind the issuance of DNR has its basis on factors related to the inherent right of people to life, medical precedent involving patients in dire medical conditions, social sentiment regarding DNR as well as religious interpretations regarding what can be regarded as an individual’s right to die. As such, the ability to write a DNR order by a doctor is thus limited by the aforementioned factors and results in a certain degree of divergence in medical practices between different countries. It must also be noted that despite the ethical basis behind a DNR order (i.e. saving a patient from more pain) a doctor cannot make such a decision unless properly empowered by the laws of the state, to do otherwise would be considered a form of medical malpractice akin to the concept of assisted suicide.
When CPR is not “futile”, but the patient wants a DNR order?
Aside from cases where CPR is futile, there are instances that do often occur where CPR can be effectively utilized in order to revive the patient, however, such an individual still requests a DNR order nonetheless. One of the reasons behind such requests is the degree of financial hardship connected with the medical costs of placing a person on life support as well as the inherent costs related to types of medications, specialized staffing requirements and an assortment of additional costs that come with maintaining an individual’s life well beyond the body’s capacity to heal itself. This is often seen in cases involving the elderly wherein they want to be less of burden on their loved ones due to the financial costs involved. One unique observation can be seen in the study of Bishop et al. (2010) where it was noted that one of the reasons behind an elderly individual asking for a DNR order was that they were already satisfied with life and that they would like to die a “natural death” rather than continue an unnatural existence through the use of various machines and methods of life support (Bishop et al., 2010: 61-67). As of late, the concept of a natural death has continued to gain ground as an inherent right to all individuals and has been the basis for the issuance of DNRs within various medical contexts since it is being classified as an inherent human right which medical institutions and governments must respect. An examination of current literature involving the right to a natural death reveals that its context is related to various instances where life is prolonged beyond what can be considered natural through artificial means of life extension. Bishop et al. (2010) explains that people should be allowed to die painlessly, peacefully and under their own terms if possible since most cultures around the world give a certain degree of importance towards the concept of death and an individual’s inevitable passing. Thus, the right to a natural death has often become one of the main factors behind the issuance of DNR orders since a person, under the opinion of Cardenas-Turanzas et al. (2011) and various other authors, should be given the choice as to when and how should they die if their end is inevitably coming (Cardenas-Turanzas et al., 2011: 45-50). In such instances where a patient invokes the right to die under their own terms the hospital must respect that individual’s wishes and implement a DNR order. In fact, it must be noted that the historical basis behind the creation of DNR orders is actually based upon the standard medical practices involving patient “death bed” requests that have developed over the years. For example, from the early 17th to 18th century it was sometimes seen that patients on their deathbeds would refuse to drink various types of medicines, aside from those that numbed the pain of their illness, since they would prefer death over the continued torment they received from their illness. In the 19th to the latter part of the 20th century when surgical techniques and blood transfusions became the norm in successfully aiding a patient’s suffering from particular maladies, it was noted that religious fundamentalism (as seen in the case of Jehovah’s Witness) which viewed blood transfusions and surgery as going against the will of God often resulted in patients outright refusing life saving surgeries. Cardenas-Turanzas et al. (2011) elaborates that it was a combination of such historical factors along with current medical practices and technologies in prolonging life that gave rise to DNR orders as they are seen today. It is based on this that it can be seen that despite the effectiveness of CPR in certain cases, the medical community has had a long and varied history of having to comply with the wishes of patients regarding their right to die and as such in instances where such a right is invoked a doctor has to respect the wishes of the patient. Before proceeding it must be noted that such instances are only applicable within a sufficient context (i.e. a patient is significantly advanced in years, suffers from a debilitating form of cancer, is in extreme pain, and has no hope of recovery as well as a variety of such circumstances). If a patient does not have sufficient context behind his/her request for a DNR then it is unlikely that it will be issued.
What if the family disagrees with the DNR orders?
In instances where a family disagrees with a DNR order, it will all boil down to whether the DNR is based on the clinical judgment of the doctor, a sanctioned DNR order from the state (though these are rare), originates from the patient prior to being immobilized and incapacitated or when a health care power of attorney has been created beforehand. Should a DNR order originate from a doctor (these are limited of course to countries that have laws that empower a doctor to make such decision), family members of the patient can contest the DNR order and are usually able to nullify it. On the other hand, if the DNR order came from a patient it cannot be revoked by either the doctor or the patient’s family members under the basic human right to “a clean death”. In such situations, both the hospital and the doctor in charge are legally obligated to follow on through with the wishes of the patient or they may face legal sanctions from the state despite the protests of the family members. Other such instances where the hands of the hospital and doctor are “tied” so to speak come in the form of a health care power of attorney which specifically states that a DNR order should be implemented when the patient is physically incapacitated and cannot make the decision himself/herself. There are certain exceptions though when it comes to a health care power of attorney wherein some states (as seen in the case of the U.S.) do not recognize living wills or healthcare proxies resulting in the need for a properly completed state sponsored form that has been endorsed by a physician for DNR orders from a pre-hospital setting (i.e. an agreement made prior to being hospitalized for whatever condition they are presently in). There are also instances where family members disagree with the DNR orders implemented by the spouse of a currently immobilized patient. One well publicized case in relation to this topic is that of Terri Schiavo who experienced massive brain damage as a direct result of a heart attack which prevented her brain from receiving oxygen well beyond the limits of recovery. While Ms. Schiavo continued to “live” she was in a vegetative state with no hope of recovery. Her husband, Michael, petitioned the local courts to have the feeding tube removed and allow her a natural death with DNR orders in place to prevent her subsequent resuscitation by the hospital staff. It was determined by the court that Ms. Schiavo would not want to prolong her life given her current status and thus mandated the feeding tube be removed. The parents of Ms. Schiavo, Robert and Mary Schindler, opposed such a decision, however, even after a prolonged and litigious appeals process the original mandate by the judge was pushed through and Ms. Schiavo was taken off life support. In such a case, it can be seen that in instances where the direct family of a patient opposes a DNR order created by the spouse, it is the immediate family in the form of the spouse whose decisions are upheld over that of the direct family resulting in the DNR order being upheld. The reverse can also be true wherein the DNR orders issued by the family can be overwritten by the decisions of the immediate spouse. State sponsored DNR orders on the other hand, as seen in the Schiavo case, are rare and can only be implemented through a process involving an immediate family member. When they are implemented even the direct family of the patient cannot successfully appeal the decision especially in cases where the spouse is involved.
What if the patient is unable to say what his/her wishes are?
There are certain situations that occur where a patient is unable to sufficiently express their wishes since they are otherwise incapacitated by blunt force trauma, a coma or a variety of other such medical conditions that prevent a person from being able to sufficiently communicate. For example, the case of Ms. Schiavo highlights how in instances where a person is unable to sufficiently communicate their desire for a “humane death” their spouse or next of kin automatically gain the responsibility of deciding whether a DNR order should be implemented order not. In instances where a state sponsored DNR order has been filed by the patient prior to being sent to the hospital it is usually the case that medical personnel have to fulfill their legal obligation and follow the specific wishes of the patient, so long as the state sponsored form has been properly filled out. Lastly, there are instances as seen in the case of the U.K. where a doctor can utilize “clinical reasoning” as the basis behind the issuance of a DNR order. It must be noted though that there is a certain gray area when it comes to implementing a DNR without the express approval of the patient due to distinct circumstances where a DNR may not be necessarily applicable. What must be understood is that the basis behind a DNR is that it is utilized as a means of ensuring a person has a more natural and humane death instead of prolonging both their hardship and that of their family through artificial means of life extension. This is normally the case seen for individuals who are suffering from cancer, have grievous injuries with no hope of recovery or are merely too old. Yet, it would be strange to apply a DNR order on an individual who is not suffering from old age, cancer, or any form of grievous injury and in fact can look forward to a long life should the proper measures be taken. For example, instances where a person has suffocated as a result of smoke inhalation or the ingestion of foreign matter which is blocking the trachea can still be revived with little if next to no ill effects. This is also applicable to instances where a relatively healthy person experiences a slight complication during surgery and would recover after some minor CPR. Thus, in such situations, regardless of the prior wishes of the patient a DNR is often not applicable. So even if an individual had entered into a DNR order prior to developing a condition that necessitates resuscitation, the fact that such a person is neither suffering from a debilitating disease, old age or grievous injury can in effect exempt the medical personnel involved from any legal repercussions despite a DNR order have been placed beforehand. It must also be noted that in certain emergency situations where EMT staff are involved it is often the case that a individual that does not want to be revive will still be revived regardless of the presence of a DNR since EMT personnel do not recognize (meaning that the validity of a DNR) is not applicable in an emergency medical situation (ex: fire, terrorist attack, drowning etc).
What if the patient lacks capacity of decision making?
Establishing that the patient was not in the right frame of mind prior to establishing a DNR request is one of the first steps behind revoking its implementation. What you have to understand is that a DNR is not implemented lightly due to the social and ethical implications surrounding it wherein up till today there still exists a certain amount of controversy in its implementation. Park, Kim, & Kim (2011) explains this by pointing out several cases involving patients suffering from a variety of psychological conditions ranging from Post Traumatic Stress Disorder (PTSD), dementia, various types of psychosis or drug induced stupors, all of which adversely affect normal thought processes (Park, Kim, & Kim, 2011: 802-813). If a patient suffers from any of the conditions mentioned or other such states which affect the normal cognitive processes of the brain then it cannot be stated that the DNR request was made by an individual in the right state of mind and can in effect be revoked by either the family, the doctor, or even the healthcare institution where the patient is at the present. On the other hand it must be noted that it is at times difficult to evaluate the mental state of an individual who requests a DNR order who has no prior recorded instance of having a psychological abnormality. For example, in one case study a patient requested a DNR after having experienced a severe poisoning which may eventually kill him. It was later found out that it was a suicide attempt and the DNR order was in effect revoked. An individual who is suicidal cannot determine whether they want to live or not, as such, they cannot be considered in their right state of mind which makes any DNR established at the time inadmissible. Other cases that should also be taken into consideration are those of patients who are mentally handicapped (i.e. suffering from a degenerative mental disorder or severe autism) wherein they cannot understand the concept behind requesting a DNR order. The basis behind a valid DNR order is that the individual who agrees to it must understand the full ramifications of what he/she is entering into, if a patient does not even realize the ramification of a DNR then it cannot be said that they are entering into it in the proper mental state which in effect nullifies any DNR entered into by this particular individual.
Once a patient has been determined as having an altered mental state that makes them unqualified as the primary decision make for a DNR order it is often the case that either the spouse or relatives of the patient make the decision as to whether or not a DNR should be implemented. On the other hand, there are instances where a person becomes mentally incapacitated due to an accident (i.e. a car crash, severe fall, etc.) which severely diminishes their mental capacity. In such instances if such an individual had entered into a valid DNR prior to being placed in such a state then that DNR is valid since it was done while the subject was still in their right state of mind.
Advance Directive
An Advanced directive is considered a form of “living will” so to speak which can take the form of a set of written instructions which created by an individual so as to direct what actions can be or should not be taken if a patient is otherwise incapacitated to make such a decision for himself/herself. It is often considered a legally binding agreement and is the basis behind the implementation of DNR orders. It must be noted though that some states within the U.S and various countries often do not recognize an advanced directive and as such its implementation is on a case by case basis.
Surrogate decision maker
A surrogate decision maker when a patient is otherwise incapacitated usually takes the form of a spouse or family member; however there are certain instances where one can be implemented based on an advanced directive or healthcare power of attorney that has been implemented beforehand under the express wishes of the client. Do note though that similar to the case of advanced directives the ability of a surrogate decision maker is only applicable on a case by case basis.
A medically futile case study
One of the best examples of a medically futile case study where a DNR order was implemented was seen in the case of Terri Schiavo who experienced massive brain damage as a direct result of a heart attack which prevented her brain from receiving oxygen. In this particular instance the patient was brain dead with no hope of reocvery whatsoever. In such an instance the continuance of further treatment and life extension would be useless since she would not be getting better anytime soon. As such, the implementation of a DNR in this particular instance could be justified.
A “full code” case study
One of the more interesting full code case studies was seen in the case of Crown Prince Nayef who died recently. Despite his failing health and the fact that reviving him was medically futile, attempts were still made nonetheless given the importance of the individual involved. From this particular example it can be seen that despite the fact that DNRs are often implemented in instances where a patient is obviously terminal there are some instances where they are not implemented or even considered at all given the importance (and in this case wealth) of the person being resuscitated.
Recognition of DNR
Introduction
In this section what will be examined is the issuance of DNR orders and the ethics behind their implementation. What must be understood is that due to the nature of a DNR order a certain set of requirements must be fulfilled before it is even applied on a case to case basis. As such this section will seek to explain the justification behind a DNR, what specific factors need to be fulfilled and the ethical backdrop from which DNR decisions are made. It is expected that by reading this section readers will be able to effectively determine which cases merit are DNR, which will not and how certain patients are selected for a DNR in the first place.
Why are DNR orders issued?
DNR orders are normally issued in cases where it has been determined that a patient has no possibility of recovery and that their current quality of life has reached a point where it would be more “humane” to allow them a more natural death given that artificial methods of respiration, nutrient intake and dealing with their various excretory processes cannot be considered a comfortable way to live. While various advocacy groups have presented numerous arguments in relation to an individual’s right to life, what they neglect to point out is that such a right applies to people who are able to live in what can be construed as a “normal” existence. Studies such as those by Baker et al. (2009) indicate that patients who are using artificial methods of life extension (nutrient systems, artificial respirators etc.) yet are able to communicate via hand gestures or writing indicate that they are under a great deal of discomfort, stress and find their current state of living almost unbearable (Baker et al., 2009: 71-76). Such a level of discomfort is of course multiplied in cases involving those suffering from severe pain as a result of their illness. Baker et al. (2009) indicates that it is actually a standard protocol within hospitals to present either the individual or their family (should the patient be unable to communicate this wishes) with a DNR order after it has been evaluated that a patient’s condition, coupled with their current quality of life, necessitates the need for a DNR. From the perspective of Baker et al. (2009) the issuance of a DNR is actually comparable to a “soft” form of euthanasia wherein instead of direct action to prevent further pain to the patient what is done instead is inaction so as to let them die naturally. Such a viewpoint has been considered controversial given the fact that it is the duty of medical personnel to care for their patient, however, Downar et al. (2011) elaborates that such an interpretation only skims the surface of what it is that a doctor must do (Downar et al., 2011: 582-587). Downar et al. (2011) explains this point by stating that the general preconception regarding medical care, medical institutions and doctors in general is that they are to provide services so as to ensure that a patient will get better. Yet, as seen from a vast majority of medical cases, not all patients get better due to a variety of factors related to old age, the progression of a particular type of cancer or disease as well as a plethora of similar circumstances. It would of course be incorrect to state that doctors and hospitals are not doing their roles, however, based on the idea that has been presented it cannot be stated that all patients who undergo medical care will get better. As such, from the perspective of Downar et al. (2011), it is more accurate to view the role of medical care, medical institutions and doctors as facilitating the”well-being” of the patient which encompasses not only factors related to treatment but also encompasses actions related to the improvement of their quality of life and pain relief of which DNR is an aspect of. It is based on this particular method of interpretation of medical care that DNR becomes a more justifiable action since from the perspective of the medical community it is a method of improving the situation of the patient, albeit in a manner that allows them to end their suffering. Another controversial aspect in relation to the issuance of DNR orders are instances involving the cost of treatments and how certain individuals and families often opt for a DNR order due financial hardship. Downar et al. (2011) goes into more detail regarding this particular issue by explaining that medical care, especially in cases involving artificial respiration, is expensive and as such from the mid 1990s till the present it can be seen that more and more people are opting for DNRs on the basis of the costs related to continued artificial life extension with no possibility of recovery. Disputes have come about as a direct result of this trend with many critics, from both the medical community and society in general, claiming that this particular precedent may result in the right to life increasingly being connected to one’s ability to pay to live. Yet, despite such accusations, the fact that families are adversely impacted by the costs associated with artificial methods of prolonging a patient’s life is an undeniable fact and as such is one of the main contributing factors behind the issuance of DNR orders. On a rather minor note, aspects related to religious notions regarding surgery, medicine and methods of artificial respiration do also impact the issuance of DNRs; however, such instances are few and far between.
Finances and DNR
One particular issue that should be delved into when it comes to DNR involves the finances of the elderly and how this impacts their decision to get a DNR. The extent for any plan for assisted care is limited by the state of its finances since daily living expenses, the price of medication, utilities and other such costs must come from somewhere. While most individuals do have retirement packages built up over several years the fact remains that such packages are at times limited. Due to this an examination must be conducted to see whether the amount of income coming from social security, investments and other forms of alternative income are sufficient to meet the needs of parents well into their 80’s and beyond. The fact is most individuals are living much longer lives as they did 50 or 60 years ago, unfortunately the current state of social security has not improved significantly since that time resulting in some individuals living well beyond what social security can provide based on the amount of money put into the system. Collopy & Friese (2010) states that “while there are alternative forms of income such as various forms of retirement packages the fact remains that factors related to inflation, economic recession and currency devaluation results in such packages becoming worth less and less as various necessities become more expensive” (Collopy & Friese, 2010: 52-57). As such these forms of income should not be considered a reliable form of income until it has been determined that they will last well beyond the expected life time of a person’s elderly parents. If such finances have been determined as being insufficient alternative means of financing cared assistance will need to be obtained till such a time that both parents are already deceased. Based on what has been presented it can be seen that any plan for caring for elderly parents must take into account aspects of financial planning, health requirements and potential services to be utilized in order to be created effectively. Furthermore, as it can be seen any subsequent form of care is inherently dependent upon the amount of finances available and as such in order to create a truly effective long term care plan from financial backing must be firmly established and created in order to ensure healthcare and various services continue to be given until the point of death. Unfortunately it is usually the case that the elderly believe that they become a financial “black hole” so to speak for their family members and as a result push for a DNR so as to lessen their burden. This is an unfortunate yet normal aspect for DNR and is one of the main reasons why they are issued within hospitals today.
Can I request a DNR order?
While any individual may request a DNR order, there are certain conditions that need to be applied before it can be considered valid. For instance, a patient must be able prove that they are in the right state of mind when asking for a DNR. Individuals that have a history of suicide attempts, have some inherent psychological disorder or are under the influence of some type of drug cannot be considered as being in the right mental state to be able to make decisions that impact whether they will live or not. Such a condition also applies to those suffering from a learning disorder or decreased mental functions as a result of an accident. Another condition that must be fulfilled is whether a DNR is applicable to a particular case. As Trunk et al. (2010) explains, any individual within the right state of mind can request a DNR, however, in instances involving either state sponsored DNR requests or those presented by a medical institution it is usually the case that there must be a valid reason behind its implementation (Trunk et al., 2010: 1719-1733). Such validation can range from a patient suffering from an incurable disease, grievous physical injury or simply old age. Without a sufficient method of validation that takes into account the concept of an individual’s “quality of life” at the present (i.e. this refers to instances involving extreme pain as seen in the case of those suffering from cancer), or their inherent right to humane death then it is usually the case that a DNR order is neither offered nor even validated despite the request of the patient. This can be seen in various instances within the U.S. wherein a DNR request had previously been requested by a patient however the state did not recognize the validity of the DNR due to the case not meriting sufficient reason for a valid implementation. It must also be noted that most DNRs that are sponsored by a state usually require a doctor to validate the request. If a doctor should rule against the claims of a patient for a DNR there is usually nothing that can be done by the patient for the request to be pushed through. The reason behind such a litigious process is due to the current ethical discourse surrounding the concept of DNR. This is due to the fact that the concept of DNR for many social groups stands at a knife’s edge between preventing the continued suffering of a person and their family through artificial means of prolonging their life and the concept of denying an individual medical care when needed.
Are DNR orders ethically acceptable?
The ethics behind issuing DNR orders lies within the gray area of moral and ethical acceptability since on one hand DNR orders help to transition patients towards the alleviation of their suffering due to a quality of life that has been adversely affected by their age, sickness or grievous physical injury. On the other hand DNR orders are seen negatively by various social groups since they in effect deny the other person the right to life. Justification for the use of DNR all boils down to the concept of the quality of life experienced by the patient and whether it would be more humane to end their suffering. For example, individuals that are considered brain dead with no hope of recovery are “technically” alive but the fact that they will never be able to walk, talk, or interact with the outside world is indicative of a state of life that would not be worth living. Various studies such as those by Baker et al. (2010) which have attempted to examine whether coma patients have a sense of awareness have shown that while there are no indicative external responses to stimuli (i.e. bodily movements) there are still distinctive cerebral processes that do occur which may be indicative of a form of “awareness” in the sense that an individual would be trapped within their own mind without the ability to see feel, or hear the outside world (Baker et al., 2010: 1349-1352). If this is so, then it can be considered more humane to allow them die since to be trapped in such a state can be comparable to a form of torture. Other such examples of an individual’s quality of life can be seen in those suffering from lung cancer, skin cancer, breast cancer and a variety of other deep rooted cancers that can cause considerable amount of pain over time. What must be understood is that while pain killers are at times effective in dulling the pain, in no way are they completely capable of removing it. There is a certain threshold between acceptable doses and levels that could kill a person which means that morphine can only work to a certain extent. Not only that a patient cannot be constantly placed under a morphine drip due to the possibility of the buildup of chemicals within their system. All of these factors equate to a person suffering from cancer normally being under a considerable amount of pain which calls into question whether it would be more humane just to let them die. While there are arguments which state that while an individual with cancer is still alive various types of treatments can still be implemented, what you need to understand is that cancer treatments which can consist of chemotherapy, surgery or even various types of chemical based treatments do not improve the quality of life of a patient but in fact make it much worse. Cancer treatments often place the body under a significant amount of strain which can either exacerbate already existing problems with an individual’s current level of health or create new complications. Not only that, the strain of the treatments often causes a significant amount of pain on the body which makes it at times unbearable for cancer patients to even be awake. When taking all these factors into consideration it can be stated that to help assist a patient out of their pain by implementing a method which will ensure a natural death can be considered as a decision in line with proper medical standards.
Ethical Issues
Introduction
When it comes to the ethical arguments behind DNR what you have to understand is that the arguments presented against it have actually been formulated as a type of ethos which specifically promotes the concept of the right to live (which most people agree with) while at the same time neglects to delve into the concept of the right to die. The concept of ethos can be described as a form of guiding beliefs that are an inherent part of a community or nations character. It is used as guide that influences a person’s behavior to such an extent that by examining the ethos behind a culture you can determine how they will react based on a given situation. It due to this that concepts behind any form of ethos must first be subjected to intense examination before it is shown to have been constructed under a proper ethical and moral framework. What must be understood is that Ethos can also refer to the way in which a person portrays themselves in an argument, in a sense that it is a method in which persuaders present an “image” to people that they are attempting to persuade. This particular “image” refers to a persuaders “character” in the sense that a person is attempting to persuade another person of the righteousness of their statements based on their inherent character. In the case of ethos it is a form of “artifice”, meaning that is created, manufactured, made, constructed etc. It can be considered a type of surface image which may in fact have an entirely fictitious relationship to what is actually true. For example, a teacher could show up in class one day wearing cowboy boots, a ten gallon hat and long sleeved t-shirt with a large image of a cactus on the front, the next day he can wear an average suit and tie while the day after that he could wear a Scottish kilt, bagpipes and one of those patterned hats. The reason I mention this is due to the fact that despite the different outfits he wears the person and the ideas that are being presented have not changed at all however what is changed is the perception of the audience regarding the idea being presented. The same can be said for ethos wherein the method in which the idea is “packaged” drastically changes the perception of the audience towards accepting the idea itself or the validity of its statements. It is in the way that it is packaged and presented to the public that changes the perception of the public to the idea that is being presented. It is this particular method of “packaging” that can clearly be seen in the case of arguments presented against DNR. It presents a one sided argument without sufficiently explaining its basis while at the same time focuses on the emotional aspects related to the so called “preservation of life”. It is this particular ethos that has been used by various advocacy groups to convince people of the validity of their claims despite the overall lack of sufficient information to justify them. An examination of the historical nature of ethos has shown that in one way or another despite the apparent ethical appearance of a certain type of ethos there is always an underlying reason behind its creation which does in fact create a beneficial effect for the individuals that created it. As it was stated earlier, ethos is not something that is inherent but rather something that has been created and manufactured with a surface image in order to fulfill a particular purpose. It is often utilized as a method of convincing people or justifying a particular set of actions and as such it is crafted in such a way so as to be convincing, believable and thus adaptable. For example when ordering someone to go into battle you do not tell them that the possibility of them dying is high rather you tell them to fight for national pride, democracy, freedom etc., even though the fact of the matter is that person will most likely die. In a sense ethos is a device utilized in order to manipulate public perception regarding truth in such a way that it promotes a particular idea on the basis of the common good but in fact it was created in order to carry out a particular action. As such, when it comes to the current arguments against DNR it is important to first examine them on whether they are based on a solid back drop of information and theory or are nothing more than a creation of a faulty ethos meant to confuse and beguile the easily fooled.
Is my consent required for a DNR order?
It is normally the case that a patient’s consent is needed for a DNR order for it be considered legally binding, however, there are certain exceptions to this rule which this section will elaborate on. The first exception occurs when the patient is incapacitated and is unable to make the decision for himself/herself. In such cases the direct consent of the patient is not required and it usually falls to the nearest relative (usually the spouse of the patient) to decide whether to implement a DNR order or not. Another exception, which has already been discussed in this paper, involves instances where a patient is not in the right state of mind to make a decision. This can occur when a patient has suffered severe damage to their cranial cavity, has been utilizing illegal narcotics or is generally considered to be suicidal. In such instances a legal proxy in the form of a family member is usually the one responsible for making the decision. Other instances where the patient’s consent is not needed occurs when local laws allow the doctor to issue a DNR order if the patient is otherwise unable to make the decision. While such instances are controversial, it is a generally accepted practice in certain countries. Aside from all the case examples provided, it is normally the patient who decides whether or not to implement a DNR order. This is due to two distinct factors: the first is the fact that people should decide for themselves whether to die a natural death or not while secondly, if it is the patient that makes the decision, this absolves the doctor from any potential lawsuits brought against him/her by members of the patient’s family.
Beneficence/ nonmaleficence
When examining the ethical principles that underlie the arguments for and against DNR it is important to explore the concepts of beneficence and nonmaleficence in order to better understand the decision making process that constitutes a DNR. First and foremost, beneficence is defined as an act that benefits other people in that it helps to prevent harm or improves the overall situation of another person. Its application in the medical field takes the form of an expectation attributed to doctors and various medical practitioners wherein they are expected to refrain from causing harm to their patient and do all that they can within their capability to maintain the health and welfare of those under their care. Non-maleficence on the other hand is the act of “doing no harm” which is one of the cornerstones of medical ethics in that a physician should not administer a form of treatment that is either ineffective, will show no benefit or has a chance of harming the patient without sufficient beneficial effects. It is the balance of beneficence and nonmaleficience that underscores the actions of all medical practitioners and is the basis for the various rules and regulations applied to the practice of medicine. It is due to such principals that the ethical basis of DNR orders are often questioned due to the fact that allowing the death of a patient goes completely against both beneficence and nonmaleficience since through inaction both the medical practitioner and the medical institution they work for would be guilt of the ultimate form of harm. To understand the basis by which DNR can still be considered ethical, it is important to understand one of the arguments which seeks to combine beneficence and nonmaleficience to justify DNR through studies which examine the mind and the concept of awareness.
When it comes to studying the brain what must be understood is that though science has enabled us to study what parts of the brain are used for a particular action it is still relatively unknown how they function and the origins of the interconnections that are responsible for the rapid fire and almost instantaneous movements that people take for granted today. For example, there mere act of typing on a keyboard involves the use of the action skill required for hand-eye coordination, the retrieval mechanisms responsible for coordinating what one needs to remember regarding the placement of the hands of the keyboard and finally the coordination of several systems involving working memory and long term memory in order to create the phenomenon known as thought which is responsible for the formation of the concepts and ideas that go into any written work. It is due to this that numerous fields of study have begun to theorize that due to our limited understanding of how the brain works it might be the case patient’s that are normally deemed as comatose, unresponsive, and have no ability to be aware of their outside environment may in fact have some sort of awareness. Theoretical studies such as those by Truog (2010 ) elaborate on this by explaining that despite an individual’s apparent comatose state the brain still functions, albeit in a reduced capacity (Truog, 2010: 84-85). Through the use of various sensors applied to the brain and certain types of external stimuli it was shown that despite being comatose a patient’s brain still had some degree of responsiveness to external stimuli as seen through various neurons activating based on the type of stimuli received. This shows that some form of “awareness” is present, however, due to the degree of neurological damage sustained through a variety of circumstances it can be theorized that such individuals are merely unable to act on the stimulation received. If the study of Truog (2010) is taken into consideration then it can be assumed that individuals that are comatose could be living in a state that is similar to the practice of solitary confinement used to punish inmates within prisons. Studies such as those by Giorgio et al. (2011) which have examined the psychological impact of social isolation reveal that even brief periods without sufficient human contact or external stimulation could result in considerable mental faculty deterioration to the point that an individual could quite literally be driven insane as a direct result of such a method of punishment (Giorgio et al., 2011: 294-298). When comparing this to the potential that people suffering from a coma could also be subject to the same condition due to a method of awareness that has yet to be pinpointed, it can be assumed that allowing them to continue living under such a state could be considered the height of cruelty. Earlier it was mentioned that beneficence is an aspect of medical ethics which utilizes the concept of “benefit to others” as the basis from which decisions in the field of medicine are derived from. Under this particular context it can be assumed that the “benefit” in the case of a DNR is perceived as alleviating an individual’s suffering through the implementation of a practice that allows them a more “natural death”. Critics against this particular method of interpreting the concept of beneficence point out that it comes dangerously close to act of euthanasia which in itself is still a highly controversial subject given that it in effect violates the act of nonmaleficience through direct action whereas a DNR order does so through inaction. Yet, based on the information presented by the Giorgio et al. (2011) study it must be questioned which is more ethical, to allow a patient to continue to suffer in a state that will slowly drive them insane, or to allow them the dignity of a humane death? Throughout this paper it has been mentioned time and time again that DNR orders are mostly applicable to cases of those who are terminally ill. It is often the case seen in such instances that the patient is suffering from a great deal of pain and discomfort and as such proponents for DNR such as Olver & Eliott (2008) state that in order to fulfill the obligations of beneficence it is necessary to interpret it outside the concept of curing a disease or ailment but rather to look at the situation from a perspective of what would create the most benefit (Olver & Eliott, 2008: 347-353). When it has already been established that a patient is terminally and nothing more can be done, it no longer becomes an issue of what process or procedure to implement in order to cure them, rather, it is more of an issue of what can be done so as to ease their passing. When it comes to artificial methods of respiration, nutrient flow and blood monitoring in cases involving the terminally ill, nonmaleficience is no longer applicable in its normal context since such actions, while perceived as “beneficial” to that patient, actually prolongs his/her suffering. As such, beneficence and nonmaleficience in the context of DNR are interpreted as easing the passing of a patient in a way that is beneficial to them while at the same time ensuring that practices which will cause them harm will not be implemented. Since prolonging a painful and degrading quality of life can be considered harmful to a patient’s well being, the concept of DNR thus becomes more ethically acceptable since it benefits the patient while at the same time alleviates their suffering. The reason why such a concept continues to be controversial lies in the fact that many mistakenly associate DNR with cases where an individual still has the potential to live a long and healthy life instead of attributing DNR to instances where nothing else could possibly be done to cure the patient. It is this mistaken correlation that continues to plague the acceptability of DNR within various medical contexts and has even led to its outright condemnation within particular cultures and societies. As technology improves it can be expected that our understanding regarding the inner workings of the brain will improve as well. It is based on this that the greatest challenge posed for understanding the concept of people having a certain degree of awareness despite being in a coma and how this will influence the implementation of DNR orders within hospital settings is not the limits imposed by present day technology (since it will improve over time) but rather the sheer amount of theoretical underpinnings in various academic fields that through one method or another attempt to highlight their processes as being the best way in interpreting what can be considered “ethical”. What must be understood is that there is a current chasm within the medical community involving beneficence and nonmaleficience and what can be considered a “proper” interpretation of such concepts.
One way of seeing this particular divergence in ideals can be seen in the separate arguments presented by Perron, de Torrente, & Morabia (2002) and Sulmasy et al. (2006) in which Perron, de Torrente, & Morabia (2002) presents that notion that it is the responsibility of all medical personnel to apply without bias or contempt the full range of their abilities in order to prolong a patient’s life or ease their suffering (Perron, de Torrente, & Morabia, 2002: 364) (Sulmasy et al., 2006: 1261-1268). However, such actions as Perron, de Torrente, & Morabia (2002) explains, should not pass into the realm of deciding whether a patient should die or not given their present condition since it could potentially lead to practices where doctors develop either a certain degree of laziness or try to “play God”. In mentioning this Perron, de Torrente, & Morabia (2002) points out various cases in India, Japan and China wherein DNR orders were often issued despite the potential for recovery for the patients. Further investigation into the matter revealed that this surge in DNR issuances was due to a combination of the doctors unwilling to perform risky surgeries which would impact their record, the fact that the patient’s family had a limited amount of assets and could not pay for the surgery and the fact that the hospital simply did not have the resources to continue the treatment without sufficient monetary compensation. While from a practical perspective such cases can be considered “understandable” given the limited resources and personnel of various medical institutions have, from an ethical perspective it can be deemed as almost monstrous since the patients are in effect valued based on the amount that can be paid for treatment. Perron, de Torrente, & Morabia (2002) explains that should DNRs become a universally accepted practice without a sufficient ethical and moral evaluation behind its implementation on a case by case basis, the possibility of declining moral and ethical standards within the medical community may come about as lax methods of DNR evaluation may be implemented so as “to keep the line moving” so to speak. For Perron, de Torrente, & Morabia (2002), such a result is unacceptable given that it would commercialize the process of medical care and would in effect increasingly reduce the importance and prevalence of the concepts of beneficence and nonmaleficience.
On the other end of the spectrum Sulmasy et al. (2006) explains that in a perfect world all needs could be met with unlimited supplies of products and services, yet we do not live in a perfect world. What is present is a state of inequality where many are denied access to necessary services and though we endeavor to provide as many as we can with affordable services our resources are being stretched to the limit as is. In matters of life or death these limitations are all the more evident especially in cases involving terminally ill patients, organ transplants and a variety of other resource and personnel intensive cases. The fact is that there are just not enough resources to go around based on the number of cases that need them. Hard choices need to be made yet these choices need to factor in not only to whom the resources can go to but rather who would benefit the most from them. Sulmasy et al. (2006) goes on to present the idea that on the one hand we have the choice of framing our decision based on an adherence to a particular set of rules in that individuals who need the resources the most (i.e. terminally ill patients or those who have suffered severe injuries). Such a method of decision making would be the most fair in terms of distributing the limited supply of resources yet it must be questioned whether such a method is truly the most effective approach. Many within the current list for resource allocation have advanced ages and may not live long while others are on the list due to conditions that they had deliberately inflicted on themselves (i.e. excessive smoking and drinking leading to cancer of the lungs and liver failure). In such cases it must be questioned whether it is moral to pick such individuals over those who are in need of medical resources through no fault of their own. There are also cases where the possibility of survival is so low that conducting an organ transplant, resuscitating them, or other similar procedures could actually be considered a waste since it is likely that such individuals will die anyway. Individuals who have many years yet to live and those who have no evidence of prior substance abuse would be able to live fuller lives and be less likely to squander the gift of life as compared to others who will most likely squander such a precious and limited gift. It must also be questioned which choice would result in the greatest degree of happiness. For individuals that have shown evidence of living longer and substance free lives the potential for generating greater degrees of happiness is that much more likely as compared to individuals that are old or are more prone to self destructive behavior. It is based on this that Sulmasy et al. (2006) advocates a program where DNRs are implemented based on beneficence in terms of who would benefit more from the utilization of hospital resources. Sulmasy et al. (2006) is quick to point out though that such arguments are not a form of discrimination against the elderly, the infirm or the critically wounded, rather, it is a factual claim based on years of examining how hospital resources are utilized and implemented.
Ethics and Ethical principals
So far this paper has elaborated on a plethora of ethics and ethical principles detailing the reasons behind the implementation of DNR orders, yet, in order to better understand their application it is important to compare such aspects to another similar case of dubious ethics employed by physicians and various medical personnel so as to show a sufficient precedent within the realm of medicine where the concepts of beneficence and nonmaleficience are interpreted in a far different manner. The science of human medicine is based on providing patients with the necessary medical advice, surgery or medication in order to help mitigate whatever malady they may apparently have. The use of placebos, while apparently sound for most doctors, is actually a form of deception since patients seeking treatment for a specific illness do so under an implicit form of trust with the doctor since they are leaving their bodies to his/her care. Such an act would normally fall under a violation of nonmaleficience since giving patients what is the equivalent of a useless sugar pill must be questioned since it is the equivalent of an ethically and morally irreprehensible practice. Based on the latest surveys conducted on most physicians, 62% indicate that they do prescribe the equivalent of placebo pills and do so under the knowledge that there is no therapeutic benefit whatsoever in their consumption and that they believe the use of placebos is a sound medical practice that will continue well into the future. The reason why placebos work despite having no medical attributes lies behind ability of the brain to influence the physical health of a person. While it has yet to be clearly understood, psychologists and various other medical professionals have studied cases where what the brain apparently believes is happening to the body actually causes it to happen despite the lack of an external force used to induce the change. The “placebo effect” is actually an extension of this line of reasoning wherein patients that are given placebo pills and told that they would be effective in helping with their malady has actually resulted in marked improvements in the overall medical condition of several patients. While initially this may not seem applicable to the case of DNR, the fact is that studies such as those by Weise (2005) have revealed that when a patient agrees to a DNR order there is a times a visible sign of relief on the part of the patient (Weise, 2005: 81-83). This takes the form of an improved quality of life where they no longer seem stressed, seem happier and apparently feel at peace. Weise (2005) explains that such a change in attitude is quite similar to the placebo effect in various patients wherein it is the belief that things will get better that actually results in a far better state of living. This is not to say that issuing a DNR will help a patient get better, rather, what must be emphasized is that by issuing a DNR a patient that is either suffering from a severe amount of patient or discomfort will realize that their pain will go away soon instead of being prolonged which in effect creates a positive psychological effect. Examples of this rather unique phenomenon in the case of placebos can be seen in individuals with chronic joint pain, back pain or other maladies related to pain. The patients describe a sudden feeling that the pain has lessened or gone away after they use placebos under the belief that the pills are actually the reason behind the loss of pain. In many cases physicians describe this as “the power of belief” wherein a patient believing that a pill will change his/her medical condition for the better actually causes a gradual improvement in overall physical health of the body. This sudden improvement has thus been connected to the state of mind of the patient wherein improving their outlook on their prognosis and being given the possibility of it improving actually creates a sufficient level of elevated mood that it helps in the recovery process In the case of DNR recipients this often takes the form of a happier and more accepting mood wherein they wait for the inevitable to come yet are at peace due to a better mental state. Similar studies have been conducted on various patients in hospitals wherein families, friends and nurses are encouraged to talk to and relate with the patient thus improving their mood during their stay at hospital. The results show that improving the mood of the patient actually drastically increases their rate of recovery or their quality of life which shows an apparent connection between moods, positive thinking and the ability of the body to recover or for pain alleviation.
Ethical Considerations
The general use of medications has created such a form of implicit trust between patients and doctors that patients always assume that by going to a hospital they will get better. As it was mentioned earlier, such a result is only limited to a certain number of cases since there are instances where a patient is too far gone for modern day medicine to work. Despite this, people still continue to go to hospitals in the hopes that something could potentially be done in order to help them. It is this very assumption that creates the feeling of expectation that results in people believing the drug will work which actually aids in the drug actually working. The same feeling of “expectancy” can be seen with various patients who take placebos and then citing that they feel better or that their condition has remarkably improved. It is this feeling of “expectation” that various advocacy groups who are against the use of placebos and DNR state as a violation of the implicit trust between doctor and patient since not only does violate a patient’s expectations of getting better but through DNR it actually results in a worse condition (i.e. death). For researchers, the ethical underpinnings utilized by such groups in their arguments are stated as being inherently flawed due to the fact that they neglect to point out the benefits gained from DNR and placebos. Yuen et al. (2011) explains that It is normally the case that DNRs and placebo are issued due to the inherent limitations placed on the physician wherein nothing else can be done in order to help the patient (Yuen et al., 2011: 791-797). For Yuen et al. (2011), it is more ethical to provide the patient with a certain “peace of mind” which would in turn benefit their condition as compared to either telling them that nothing can be done or that their suffering will be prolonged until they subsequently die. What you have to understand is that the psychologically beneficial effects from the utilization of placebos and DNR is actually the result of the Pavlovian conditioning process wherein people are conditioned to expect a certain response when an appropriate stimulus is given. Take for example the case of a cat and a lab assistant, a lab assistant can come into a room wearing a bright orange shirt and use an air horn on the cast in order to scare it. Moments later the same technician comes into the room this time wearing a blue shirt yet bringing the cat some food. Continuing this process over a period of several weeks will actually cause the cat to experience anxiety whenever it sees the color orange while adversely the cat will appear calm, relaxed and expectant whenever it sees the color blue. This same level of conditioning is already apparent in society wherein people who have taken all sorts of medications throughout their lives for a variety of causes have already embedded the expectation in their minds that taking medicine that is told will work for their illness will actually work. As a result of this conditioning process, placebos that should not have any effect whatsoever on the condition of a patient actually stimulates a certain mental response which associates the placebo as something which will help the body which actually creates a biological response that results in an improved condition for the patient. While the results may vary from patient to patient depending on the claims of the doctor it has actually been shown that nearly 32% of the population in the United States is actually vulnerable to the mechanism behind expectation and conditioning which would make them susceptible to the use of placebos. In the case of DNRs the same effect is at work wherein the Pavlovian mechanism of reinforcing that their pain will go away soon (once they die) actually results in a certain positive psychological effect which actually results in a certain degree of pain relief. This was seen by Silveira, Buell, & Deyo (2003) in his examination of elderly cancer patients and their wish for a DNR order (Silveira, Buell, & Deyo, 2003: 1435). Once a DNR was implemented and the patient’s knew that their pain would end soon this resulted in them supposedly feeling better and actually contributed to the psychological well-being of the patient’s family members as they saw that the patient actually looked at peace and was pain free. It is due to instances such as these that further reinforce the arguments for the use of DNR as an ethical form of relieving a patient of their pain due to their current quality of life.
Justification for using Placebos and DNR
There are three primary reasons behind the use of placebos and DNRs: cases where normal medication would be useless, cases where the problem is all in the patients head and finally cases where the patient cannot afford the necessary type of medication that would actually work. Placebo treatments have been used in a variety of treatments where modern medicine has yet to actually provide cures. These range from Crohn’s disease, Parkinson’s disease, various forms of cancer, and even erectile dysfunction. Due to the expectation and conditioning response evident in a large percentage of the population, patients who have nearly incurable cases by medical standards actually do start to feel better after the use of placebos and after the issuance of DNR orders. There is noted improvement in overall health, appetite and physical performance. Even cases involving extreme cases of pain where no apparent pain killers work have been shown to actually lessen the degree of pain to an extent due to the belief of the patient in the use of these kinds of pills or in the fact that they will die soon. There are certain cases that apparently defy all medical examination where a patient has certain symptoms or levels of pain that apparently do not have any medical cause whatsoever. In such cases placebos are usually given in order to determine whether there is actually any pain or if the patient is merely trying to get a prescription to addictive forms of pain medication such as Vicadin. Lastly, in the case of several communities throughout the U.S. there are various individuals suffering from ailments who cannot afford to buy normal types of medication due to their economic situation. As a result some doctors prescribe placebo pills to these individuals as a means of easing whatever symptoms they may have till a more affordable solution can be attempted. In other such instances DNRs are also reluctantly issued by medical personnel which does present a certain degree of ethical repugnancy since the type of medical care issued should be based on what one can pay, however, given the limitations of hospital resources it is at times understandable that the hospital cannot make exceptions for all cases. The problem though is the practice of placebo usage and DNR implementation is still based on violating the trust between doctors and patients. In cases where the patients were informed after placebos proved to be effective that they were actually on the placebos the result was usually an immediate regression towards their old symptoms. This shows that placebos cannot be used a permanent solution in some medical cases. On the other hand their continued beneficial use is evident and as such justifiable in light of the needs of particular patients. The same can be said in the case of DNR wherein the positive psychological effect of the DNR implementation actually hinges on the belief of the patient that their suffering will end. If they are still revived despite the DNR order in place it is often the case that they will regress into a more painful and uncomfortable state due to the realization that their suffering will be prolonged. The best way to handle such situations is to regulate the prescription of placebos and DNRs to such an extent that doctors do not regularly hand them out just to get rid of patients but rather use it as a method of last resort in order help patients deal with what ails them.
Autonomy
Understanding the need for Corporate Social Responsibility and its integration into values and ethical standpoints
On average people consider their ethical standpoints as an unshakable attribute by which they determine the inherent rightness or wrongness of a particular set of actions however one inherent problem with this is that a standpoint is based on the point of view of each unique individual resulting in a veritable plethora of views, opinions and standpoints. For me, the basis of my values and ethics is one that requires an incorporation of corporate social responsibility into my decision making process in order to properly evaluate the ethicality of my decision. This is not to say that I use CSR (corporate social responsibility) as an everyday method of evaluation, instead, I use it as a method that takes into account the ramifications of my actions on customers and clients. The reasoning behind this is based on the idea that what is ethically dubious for one individual is ethically sound for another. Take for example the case of Glacéau, a subsidiary of the Coca Cola Corporation, their line of business deals in the sale and distribution of vitamin water, a supposedly healthy beverage choice for people that want to incorporate more vitamins into their daily diet. Studies into the properties of vitamin water have shown that not only does it contain 32 grams of high fructose corn syrup which has been connected to rampant obesity but the supposed nutritional value of the vitamins in the water have been proven to be mostly ineffective since the populations that the company is marketing the drink to (mostly U.S. consumers) have been shown to possess more than adequate amounts of vitamins in their system. In fact the product itself has been shown to be more detrimental rather than beneficial to a person’s health due to the large content of sugar and chemicals present in the water. Yet Glacéau continues to market the product under the claim that it will improve a person’s health and is beneficial towards a healthy lifestyle. The continued marketing campaign of the company not only is a violation of the standards of corporate social responsibility but also endangers consumers since many of them might use vitamin water as a replacement for actual water and as a result endangers their health. As a future member of the medical community I have to think of not only the ramifications undesirable medical practices have on the reputation of the company but also how they affect ordinary consumers. It is due to this that my personal code of ethics in any of the medical practices that I enter will be based on the concept of corporate social responsibility wherein the organization will ensure its actions create a positive impact on consumers, employees and markets under fair and ethical business practices. My own personal values in future medical decisions will be guided under the concept of normative ethics where before I proceed with any decision I will determine whether what make my action right is actually based on an unbiased ethical viewpoint. For the managers at Glacéau, their marketing of vitamin water is for them ethically sound since it provides a means of income for the company yet such a standpoint is ethically dubious since the potential results could possibly endanger people. It is due to this that personal values cannot be truly trusted, as such, deep introspection must first be accomplished before any decision is undertaken in order to determine whether the decision made is ethically sound both for me and other people.
Justice
It is at times strange to consider that the concept of justice has any relation whatsoever to DNR, however, despite the relative amount of disparity between the two concepts there is a certain degree of interrelation between the two. From the perspective of Baker et al. (2003) the concept of justice applies to cases of DNR when it comes to instances where an individual is being subject to the death penalty (Baker et al., 2003: 343-349). Obviously this particular individual should not be revived since the punishment for their crimes is death. As such, in this particular the concept of “justice served” overrules the necessity of reviving an individual and exempts the practice of DNR from the normal ethical guidelines and underscore its use.
Other ethical principals
Importance of Ethics Training within the Medical Community
This section delves into why there is a distinct lack of ethical behavior within the medical community at large and what can be done in order to resolve such an issue.
The article “Ethics Training and Businesspersons’ Perceptions of Organizational Ethics” by Sean Valentine and Gary Fleischman is an investigation into the influences of corporate culture, ethical codes of conduct and ethics training into the level of job satisfaction, performance and ethical practices that employees bring to the workplace. Through a combination of extensive academic research and the use of a questionnaire in order to evaluate the opinions of a select group of employees who are often faced with ethical decisions on a daily basis, the researchers were able to present the importance of ethics training as a means of encouraging and facilitating proper ethical practices within the workplace. Furthermore, they indicated that ethics training allows a workforce to be more aware of the ethical codes of conduct that a company abides by and as a result enables them to be far more likely to conduct themselves in a manner that is in line with the highest standards of moral and ethical behavior. The reason this is being brought up is due to the fact that studies such as those by Eliott & Olver (2011) have shown that there has been an increasing lack of ethics within the field of medicine which is in part due to a certain degree of neglect on the part of medical institutions in sufficiently training their employees in various ethical practices (Eliott & Olver, 2011: 147-158). As Eliott & Olver (2011) explains, that even the best medical institutions with the highest standards of internal ethical practices fail to implement methods of training and instead rely upon the established rules and regulations set forth by the hospital administration. Eliott & Olver (2011) states that this is an insufficient and impractical method of ensuring ethical standards since to rely on rules alone instead of constant education and reminders is the height of folly.
The study also happens to place a considerable emphasis on the influences of organizational culture and how even organizations with the best ethical codes in the world often all prey to instances of unethical conduct within its ranks. In order resolve such issues Valentine and Fleischman recommend the use of ethical training sessions as a means of building up on the framework of actions initially established by the ethical codes of conduct emphasized by the company. They state that ethical codes are not enough to dissuade unethical actions, it is often necessary to create an even greater emphasis on ethics in order for employees to feel the correlation between ethical action and the company culture that they are a part of.
Theoretical issues identified in the article
The main theoretical underpinnings of the study is the concept of ethical training and existing ethics codes being the best way in order to ensure ethical actions among the employees of a company. Such a theory has been backed by various studies such as those by Torke et al. (2011) which explain that by creating an environment where employees are constantly exposed to ethically progressive ideas, notions and behaviors, eventually they will be influenced in the same fashion (Torke et al., 2011: 1326-1311). This theory addresses the “social notion” behind working within an organization by creating the impression that since everyone within the company is following and advocating the use of ethical behaviors then as an employee of the company a person should also implement such aspects into the work that he/she does. One problem with this way of thinking is that it is far too naïve in that there are other factors that influence the way in which an employee becomes ethical or not. This can come in the form of job satisfaction, salary, career growth, belief in the mission statement of the organization as well as other such factors which influence the behaviors of an employee. No matter how much ethical training a person receives or no matter how exacting a company’s code of conduct are, such factors can only be considered as secondary contributors to enabling a person to develop ethical ideas but in no way does it influence an individual into avoiding all unethical behaviors. The theory presented by Valentine and Fleischman also happens to correlate the concepts of job satisfaction with ethics wherein through ethical training and learning that the company you work for has an ethical code of conduct this would in turn increase an individual’s overall level of job satisfaction. The inherent problem with this type of theoretical basis is that that job satisfaction has very rarely been correlated with ethics, rather, it has been shown time and time again that having an employee become satisfied with their job often involves developing interest, creating role variability and ensuring that they are paid adequately. While there have been some theorists who have stated that job satisfaction is often connected to the ethical structure behind the job itself, they are mostly in the minority and as such calls into question the validity of the theoretical basis of the article.
Analyzing the article
Based on what I have learned about medical ethics I have to say that the authors of the article do have a valid point when it comes to ethical codes of conduct and ethical training being influential factors in helping employees become more ethical. The fact is that ethical behaviors from employees are influenced by the medical culture and the corporate environment that they are exposed to. The more ethically oriented the medical culture and corporate environment is, the more likely employees are to display ethical behaviors. The reverse is also true wherein the more unethical the environment the greater the potential for employees to show unethical behaviors. This was seen in the case of India wherein Puri (2006) showed that gendercide (the act of systematically killing of an unfavored gender such as females while in the womb) was prevalent with the local medical culture being to blame for the various methods and procedures being made available to the general public so as to create a culture of abortion (Puri, 2006: 35 – 39). Another aspect of the article that necessitates a considerable degree of examination is the assumption of the researchers that a well structured ethical code of conduction and ethical training will result in ethical actions by the institution as a whole. While it may be true that such assumptions have been backed up by a considerable degree of research that they presented, modern day examples of unethical practices by companies show an entirely different story altogether. High ranking employees of Wal-Mart and GE have been embroiled in the news as of late due to a series of considerably unethical actions which have captured the attention of the media. In the case of Wal-Mart this involves a series of bribes to Mexican officials in order to expedite the expansion of the company in Mexico. The GE employees on the other hand were part of an apparent insider trading scheme. It is this and several other examples of companies that pride themselves on their code of ethics and their ethical training that makes the assumptions of Valentine and Fleischman increasingly questionable. Such actions though can be regarded as merely being isolated to a small percentage of the employees within that company and is actually not endemic within their organizational structure. Unfortunately, when examining the use of the bailout money given to such companies in 2009 in order to help facilitate further growth within the U.S. economy, these companies merely utilized the funds in order shift their manufacturing operations to other countries such as India and China. While it is technically legal, it is both ethically and morally irreprehensible since it was the intent of the government that such funds be utilized in order to create more jobs within the local economy instead of facilitating actions that would hamper recovery efforts even more. Thus from this particular perspective it can be seen that even if ethical codes of conduct and ethical training sessions are implemented to create ethical employees, this does not mean that the end result will create an ethical company. The problem with the article is that it relies too much on ethical codes of conduct being a sufficient structure to influence a business culture within a company. From the perspective of Feen (2010 ), even the most ethical of employees with the best code of ethics and ethical training possible can fall prey to unethical actions within a medical culture when it concerns either the performance of the department or the necessity of implementing measures connected to competitive survival (Feen, 2010: 80-81). This was seen in the case of the outsourcing industry wherein many companies outsourced various aspects of their operations to other countries such as India and China. On the surface such companies stated that they stuck to the strict environmental rules and regulations established by the EPA within the U.S., however, since such regulations do not apply to outsourced operations in other countries these companies can in effect flagrantly degrade the environment through their operations while still stating that they were not the ones directly responsible for the incidences, rather, it is all the fault of one of their suppliers. This is just one of the numerous examples of corporate double standards that exist in organizations that supposedly have high ethical codes of standards and undergo ethical training sessions. Another problem I had with the article was that it stated that company leaders should place greater emphasis on employee job attitudes as one of the method of managing the issue of ethics within an organization.
Identifying the gaps
When it comes to employee retention and performance, job satisfaction is the deciding factor behind such principles of corporate human resource development and as such should be examined from a multilevel perspective in order to ensure employees continue to perform adequately and stay longer with the company. In the case of the article, it is shown that the researchers correlated job satisfaction with a greater understanding of an organization’s ethical underpinning and being able to better relate to the ethical codes of the organization. The authors state that by realizing the institution that they work for has distinct ethical standards, this in turn results in a far more likely result of employees acting in a moral and ethical fashion while at the same time having a greater degree of job satisfaction. The inherent problem with such a concept is that researchers such as Jaya & Liew (2012) explain that while there are many ways in which job satisfaction can be accomplished ranging from new orientation methods, mentoring, continuous job training developments and other such factors it is normally the case that ethical codes and ethical codes of conduct do not act as a means of creating greater degrees of job satisfaction among a company’s employees (Jaya & Liew, 2012: 488). The main reason behind is due to the fact that job satisfaction is often linked to the amount of interest derived from doing a particular task. The greater the degree of interest the more likely it is that people will like their job. Evidence of this can be seen in the case of employees who dislike their careers despite having large salaries since they have lost all interests in doing their job. Ethical considerations can be considered a secondary contributing factor to job satisfaction, in no way though can it be attributed as being one of the main reasons behind a person enjoying their job. It must also be noted that while the study was able to get the opinions of various employees via questionnaires, it neglected to sufficiently indicate how organizational culture also plays a distinctive factor in influencing ethical behavior. While such a factor was mentioned, it was only done briefly and as such is indicative of a gap in the literature which is rather important as seen in the case of this evaluation which showed just how much organizational culture and worker environments influence the ethical function of an organization as a whole and not just through its individual employees.
Assess the conceptual differences and similarities when applied to the context
There is an old saying that states that “the left hand doesn’t know what the right hand is doing”, in the case of medical institutions this takes on a more significant meaning due to the proliferation of various departments, operational sites and standards of medical practices in particular areas. Not all departments actually know what other departments are doing and as such this leaves a great deal of ambiguity as to what sort of ethical practices particular departments are or are not engaging in. As such, this presents the necessity of establishing a standard set of ethical practices and procedures across all departments due to the need to ensure that when represented by a particular department in a certain medical venture their ethical practices do not reflect badly on the rest of the company. What must be understood is that when a particular operation, department or employee engages in a distinctly unethical practice this makes patients think of the hospital as a whole as being unethical despite the action being isolated to that particular instance. It is based on this particular example that there needs to be a certain code of ethics in order to ensure a generalized form of ethical accountability across all departments in order to prevent any action that might jeopardize hospital’s image. From a certain perspective though, it can be stated that ethical codes and ethics training does help to facilitate better ethical behavior, however, as Jaya & Liew (2012) explains while such actions help to ensure that individual employees think ethically this does not outright prevent unethical actions from the company itself. Jaya & Liew (2012) elaborates on this by stating that the best way of preventing a hospital from conducting unethical actions is to implement proper methods of ethical evaluation and overseeing the actions of the hospital itself. At times this involves the creation of a separate department within the hospital whose main purpose is to evaluate the ethical actions of the organization and propose suggestions which are in line with widely accepted ethical procedures and practices.
Organizational Evaluation
One example that should be taken into consideration when it comes to proper work place ethics is the company, Convergys. As a company whose line of business lies in outsourcing the customer service departments of various multinational corporations Convergys places an emphasis on workplace ethics because employees deal with the complaints and concerns of various customers day in and day out which require a certain ethical fortitude. The inherent business culture of the company centers itself around the development of employees as being part of teams with each account floor being separated into 13 teams of ten individuals each. It is the belief of the company that by creating a sense of camaraderie and friendly competition between the various teams that this would in turn contribute to a more effective operational output. The vision/mission statement of the company is to outthink and outdo the competition by providing the best services for its clients using sound business practices. The code of ethics of the company centers on the development of individual workers to their full potential, the company does not count workers as merely a number on a sheet but considers them an important resource to be developed. As such the company’s code of ethics encourages managers and team leaders to treat even the lowliest employee as equals in order to foster an open environment where ideas are easily exchanged in order to improve business practices. The reasoning behind this particular organizational structure lies with the fact that the customer services industry is actually a high churn market with employees entering and leaving companies at a rate much higher than in other industries. Companies seek to retain more employees that they loose and as a result have had to change ethical and value standards in order to encourage employee retention. The reason this has been brought up is due to the overly high burnout rate seen in the medical community today. This is due to a combination of job pressures, patient deaths as well as an assortment of other instances which place a significant amount of stress on hospital staff. This often results in various instances where distinctly unethical practices are implemented as a direct result. This at times leads to the issuance of DNRs since the staffs at a hospital are far too burned out to be able to successfully deal with the patient’s case. As such, it is recommended that in order to help resolve such an issue in various medical organizations that they implement the same methods utilized by Convergys so as to create a better working environment which would result in far fewer rates of employee burn out.
Legal Issues
Introduction
Earlier it was mentioned that the laws applicable to DNR are different based on either the state, country or cultural backdrop from which the decision to apply or not to apply a DNR are based upon. While there is a certain universality to particular medical practices, the fact that the concept DNR is applied differently in different bodes further investigation as to why this is so. To better understand the points of conflict in this particular case realism will be utilized in order to examine the actions of the states involved and determine why they pursued a particular action the way they did. First and foremost, for realists cooperation between states (states refers to different countries in this particular context) is difficult due to the possibility of cheating and the concept of relative gains between different classes of states while from a liberalist perspective cheating does also occur however instead of relative gains what occur are collective actions problems. From this particular perspective it can be seen that since there is an inherent level of difficultly for states to establish a method of cooperation then it is plausible to assume that differences would of course occur in certain aspects related to generalized practices involving methods of healthcare, especially on controversial issues such as DNR which is normally influenced by aspects related to religious fervor and cultural tradition.
While the easiest solution to this problem would be to simply enact some form of regional cooperative agreement all the parties involved have been hesitant if not unwilling to enter into a proper arrangement despite the fact that the conflict of interest in this particular case is one that is merely perceived and not wholly substantiated based on solid evidence.
Taking the liberal view into consideration, collective action problems for interstate cooperation can be surmised into 2 distinct problem sets, namely:
- Achieving cooperation between states is relatively costly to organize, monitor and enforce.
- There is the possibility of “free riding” wherein certain states benefit from the cooperation but do not pay the costs of achieving cooperation.
From the realist perspective even if states found themselves in a situation where cooperative action would be mutually beneficial the fact still remains that these states are still concerned over the concept of relative gains that would result from cooperative action. Based on this, realists state that cooperation is a lot more difficult to achieve than otherwise believed due to the behavior of states where they would give up the potential gains accrued through cooperation if such cooperative action resulted in greater gains for other parties in the cooperative agreement. What must be understood is that there is mutual distrust between the parties involved which is fueled by assumptions that the other the other will use particular issues (such as DNR) to unduly influence the internal decision making capabilities of the state. It is based on this that it is implausible to believe that there will ever be a generalized method of DNR application given the various problems in interstate cooperation presented.
United states Laws
When it comes to laws regarding DNRs in the context of U.S. based laws it can actually be seen that there is a considerable degree of complication involved given that DNR orders are interpreted differently depending on the state in question. For example, while certain states acknowledge living wills and DNRs prior to hospitalization others do not. This of course has led to considerable confusion within the U.S. especially when taking into consideration the number of advocacy groups against DNR.
United Kingdom Laws
In the case of the U.K. there is a more generally accepted version of DNRs wherein it is up the decision of the attending physician whether a DNR order can be applicable to a certain individual.
Kingdom of Bahrain Laws
The Kingdom of Bahrain on the other hand follows Islamic law when it comes to DNR and as such aspects regard this will be elaborated on in the succeeding section.
Religious Considerations
Introduction
The following section will elaborate on the various religious considerations that impact DNR in the context of Islam. It is expected that after reading this section readers will be enlightened as to how religion impacts the way in which a DNR is implemented and how public relations and propaganda are utilized by religions to solidify their views regarding DNR.
Definition of death in Islam
An examination of the traditional criteria for death under Islamic law reveals that death was originally construed as occurring after the complete cessation of an individual’s respiration and circulation. Due to subsequent advances in medical technology such a method of evaluation has gone through several new iterations as direct result of technologies related to artificial respiration and blood circulation. The current method of evaluation now consists of examining comatose patients on the basis of brain death. In this particular instance an individual is declared legally dead after 3 credible physicians have examined the body and state that there is significant irreversible damage to the brain to the extent that they are considered brain dead. It is at this point that the body is considered a corpse which is merely being maintained by artificial methods of preservation. It is at this point that the body is at times slated for organ donation with the various machines utilized in keeping it “alive” turned off. As it can be seen in this particular instance, Islamic law differs greatly from laws seen in the U.S. and the U.K. since the concept of DNR is applied after an evaluation declaring an individual a corpse despite the body being “technically” alive. Lo et al. (2010) attempts to explain why such a practice is in place despite mostly negative public perceptions by indicating that through a combination of religious law and government edict, it becomes almost impossible to overrule such a decision given the sheer amount of influence and control both Islam and the local Muslim government have in the lives of the local populace.
Islamic principals
The following is an elaboration on the Islamic principles that are applicable to cases involving DNR. First and foremost it must be noted that DNR is normally not permissible under Islamic law unless in certain cases involving the following instances. The first instance involves a case where a sick person has been taken to a hospital and is pronounced dead on arrival. In such a case it is obvious that there is no need to use resuscitation equipment and as such a DNR is no longer necessary. The second instance consists of an evaluation of a patient’s condition on whether or not it fit for resuscitation according to the opinion of three trustworthy specialist doctors, in which case there is also no need to use resuscitation equipment and a DNR order is implemented. Third case consists of an examination of a patient’s sickness on whether it is chronic and untreatable, and if death is inevitable according to the testimony of three trustworthy specialist doctors, in which case there is no need to use resuscitation equipment and a DNR is immediately implemented. The fourth instance is slightly controversial since it involves the case of an individual that is still technically alive however is considered a “vegetable”. The forth instance consists of a patient that is incapacitated, or is in a persistent vegetative state and chronically ill, or in the case of cancer in its advanced stages, or chronic heart and lung disease, with repeated stoppages of the heart and lungs, and three trustworthy specialist doctors have determined that, then there is no need to use resuscitation equipment in which case a DNR is implemented despite the individual being “technically alive”. The fifth instance where a DNR is applicable is instance where there is any indication in the patient of a type brain injury that cannot be treated according to the reports of three trustworthy specialist doctors (Lo et al., 2010: 436-442). If the patient has been evaluated as such, then there is no need to use resuscitation equipment, because there is no point in doing so. The last instance involves an evaluation of whether reviving the heart and lungs is of no benefit and not appropriate because of a certain situation according to the opinion of three trustworthy specialist doctors, then there is no need to use resuscitation equipment, and no attention should be paid to the opinions of the patient’s next of kin concerning the use of resuscitation equipment or otherwise, because this is not their specialty as stated by Islamic law.
Overview of cultural and religious case issues
In the realm of public relations your ability to influence the way people accept and interpret information is directly related to your success or failure in any endeavor in this particular field. In relation to this persuasion is the ability to get people to do what you want and make them feel that it is in their best interest to do so. In a way persuasive messages can be considered the engineering of consent, wherein people are convinced of the validity behind certain actions through the creative use of words and phrases. This is the case often seen with cultural and religious case issues wherein persuasive reasoning it utilize as a tool in order to bend public opinion towards a particular way of thinking. Persuasive reasoning influences their behavior to such an extent that it creates consent for the action being undertaken. In a way it is a manner of communication which imparts a specific message with the intent of facilitating a certain action to be accomplished. Wilcox states “perception is interpreted as being used in the following manner: to change or neutralize hostile opinions, to crystallize latent opinions and positive attitudes, and finally to conserve favorable opinions”. In the case cultural and religious issues and the way they either vilify or uphold DNR, it can be states that the importance of persuasion to successful contemporary public relations all boils down to its ability to influence individuals towards a certain train of thought. As such it can be stated that persuasion shapes perceptions and thus the way people interpret and accept information. Which why in certain countries it can be seen that there variances in the way in which they interpret the concept of DNR. What you have to understand that is that religious often utilize propaganda as a means by which they influence the thoughts and actions of individuals without having to utilize verifiable evidence to support such claims. Propaganda is a method of communication which is used to influence the attitudes of specific groups of individuals towards a particular cause or position. In essence, instead of a sense of impartiality propaganda actually presents information in such a way so as to influence an audience through selective dissemination of information in order to create an emotional rather than a rational response to certain issues (Katsetos & Mirarchi, 2011: 629-632). For example in the case of the Australia’s cancellation of the Fuel Watch program Senator Xenaphon utilized propaganda stating that Fuel Watch was not an effective means of helping consumers stating the need to tackle the big four oil companies using another method, what most people fail to notice is that he omits the details the successes the Fuel Watch program actually had which indicates possible ulterior motives on his part. His actions resulted in the end of the National Fuel Watch scheme which to an extent could be considered a step back from giving consumers more control over how they purchase gasoline. What must be understood is that propaganda utilizes elements such as loaded questions, partial synthesis or even lying by omission in order to gain the desired response. One use of effective propaganda can be seen in the online article “Cultural Cringe where the writer selectively introduces facts which lambasts and derides the Australian video presentation for its World Cup 2022 bid. Throughout the article there is little mention of the creativity that went into the video, the unique approach that Australia took or the overwhelming positive response viewers had for the commercial, rather, what is mentioned is nothing more than a continuous tirade focused against commercial itself. It must be noted though the use of the term propaganda, as stated by Wilcox, has been connected to falsehoods, lies and deception. It is true though that propaganda used by various PR departments have been utilized in various anti DNR campaigns as a form of sociological warfare where detrimental facts on the process are released to the general public. On the other hand propaganda is also used in various public information campaigns by governments for positive effects such as the Australian governments fight against illegal downloads connoting their use with stealing and its use by the U.S. during the invasion of Afghanistan and Iraq as a supposed “war on terror”. In essence the use of propaganda and its effects can be associated with the ethical reasoning behind its usage. Unfortunately under the context of religious cultural case issues involving DNR it is often the case that negative rather positive propaganda is utilized.
Conclusion and Recommendations
Conclusion
Based on the sheer amount of data that has been presented in this study it can be stated that despite the ethical arguments against DNR, the fact that it enables an individual to have a natural death and frees them from their discomfort and pain makes it an acceptable medical practice based on its positive effects. Even with the various ethical arguments against its implementation this study has proved that such arguments are often times based on false ethos and propaganda that lacks a sufficient basis from which they could even be marginally justifiable when set against the sheer amount of beneficial effects that DNR has.
Recommendations
As seen within this study numerous methods of recommendation have been stated involving the implementation of ethics training, organizational change and a variety of other practices that should improve the ethical basis of the modern day medial community. It is expected that should such improvements be implemented there would be fewer cases of ethical mismanagement especially in the case of DNR.
Reference List
Bacchetta, M, Eachempati, S, Fins, J, Hydo, L, & Barie, P 2006, ‘Factors Influencing DNR Decision-Making in a Surgical ICU’, Journal Of The American College Of Surgeons, 202, 6, pp. 995-1000, Academic Search Premier, EBSCOhost.
Baker, J, Rai, S, Wei, L, Srivastava, K, Kane, J, Zawistowski, C, Burghen, E, Gattuso, J, West, N, Althoff, J, Funk, A, & Hinds, P 2009, ‘Race Does Not Influence Do-Not-Resuscitate Status or the Number or Timing of End-of-Life Care Discussions at a Pediatric Oncology Referral Center’, Journal Of Palliative Medicine, 12, 1, pp. 71-76, Academic Search Premier, EBSCOhost.
Baker, D, Einstadter, D, Husak, S, & Cebul, R 2003, ‘Changes in the Use of Do-not-resuscitate Orders After Implementation of the Patient Self-determination Act’, JGIM: Journal Of General Internal Medicine, 18, 5, pp. 343-349, Academic Search Premier, EBSCOhost.
Baker, J, Kane, J, Rai, S, Howard, S, & Hinds, P 2010, ‘Changes in Medical Care at a Pediatric Oncology Referral Center after Placement of a Do-Not-Resuscitate Order’, Journal Of Palliative Medicine, 13, 11, pp. 1349-1352, Academic Search Premier, EBSCOhost.
Berger, JT 2003, ‘Ethical Challenges of Partial Do-Not-Resuscitate (DNR) Orders: Placing DNR Orders in the Context of a Life-Threatening Conditions Care Plan’, Archives Of Internal Medicine, 163, 19, p. 2270, Academic Search Premier, EBSCOhost.
Bishop, J, Brothers, K, Perry, J, & Ahmad, A 2010, ‘Reviving the Conversation Around CPR/DNR’, American Journal Of Bioethics, 10, 1, pp. 61-67, Academic Search Premier, EBSCOhost.
Cardenas-Turanzas, M, Gaeta, S, Ashoori, A, Price, K, & Nates, J 2011, ‘Demographic and Clinical Determinants of Having Do Not Resuscitate Orders in the Intensive Care Unit of a Comprehensive Cancer Center’, Journal Of Palliative Medicine, 14, 1, pp. 45-50, Academic Search Premier, EBSCOhost.
Collopy, K, & Friese, G 2010, ‘HOSPICE and DNR care’, EMS Magazine, 39, 8, pp. 52-57, International Security & Counter Terrorism Reference Center, EBSCOhost.
Do Yeun, K, Kyoung Eun, L, Eun Mi, N, Hye Ran, L, Keun-Wook, L, Jee Hyun, K, Jong Seok, L, & Soon Nam, L 2007, ‘Do-Not-Resuscitate Orders for Terminal Patients with Cancer in Teaching Hospitals of Korea’, Journal Of Palliative Medicine, 10, 5, pp. 1153-1158, Academic Search Premier, EBSCOhost.
Downar, J, Luk, T, Sibbald, R, Santini, T, Mikhael, J, Berman, H, & Hawryluck, L 2011, ‘Why Do Patients Agree to a ‘Do Not Resuscitate’ or ‘Full Code’ Order? Perspectives of Medical Inpatients’, JGIM: Journal Of General Internal Medicine, 26, 6, pp. 582-587, Academic Search Premier, EBSCOhost.
Eliott, J, & Olver, I 2011, ‘Dying cancer patients talk about physician and patient roles in DNR decision making’, Health Expectations, 14, 2, pp. 147-158, Academic Search Premier, EBSCOhost.
Feen, E 2010, ‘Leave Current System of Universal CPR and Patient Request of DNR Orders in Place’, American Journal Of Bioethics, 10, 1, pp. 80-81, Academic Search Premier, EBSCOhost.
Giorgio, G, Nicoletta, C, Manuela, C, Francesca, C, & Serena, R 2011, ‘The Pseudomonas aeruginosa DNR transcription factor: light and shade of nitric oxide-sensing mechanisms’, Biochemical Society Transactions, 39, 1, pp. 294-298, Academic Search Premier, EBSCOhost.
Gouda, A, Al-Jabbary, A, & Fong, L 2010, ‘Compliance with DNR policy in a tertiary care center in Saudi Arabia’, Intensive Care Medicine, 36, 12, pp. 2149-2153, Academic Search Premier, EBSCOhost.
Hite, CA 2000, ‘THE DO-NOT-RESUSCITATE DECISION: THE CONTEXT, PROCESS, AND CONSEQUENCES OF DNR ORDERS’, Death Studies, 24, 4, p. 307, MasterFILE Premier, EBSCOhost.
Jaya, H, & Liew, Y 2012, ‘Why Not DNR?’, Journal Of Palliative Medicine, 15, 4, p. 488, Academic Search Premier, EBSCOhost, viewed 24 May 2012
Katsetos, A, & Mirarchi, F 2011, ‘A Living Will Misinterpreted as a DNR Order: Confusion Compromises Patient Care’, Journal Of Emergency Medicine, 40, 6, pp. 629-632, Academic Search Premier, EBSCOhost.
Lo, Y, Wang, J, Liu, L, & Wang, C 2010, ‘Prevalence and Related Factors of Do-Not-Resuscitate Directives Among Nursing Home Residents in Taiwan’, Journal Of The American Medical Directors Association, 11, 6, pp. 436-442, Academic Search Premier, EBSCOhost.
Lyon, M, Williams, P, Woods, E, Hutton, N, Butler, A, Sibinga, E, Brady, M, & Oleske, J 2008, ‘Do-Not-Resuscitate Orders and/or Hospice Care, Psychological Health, and Quality of Life among Children/Adolescents with Acquired Immune Deficiency Syndrome’, Journal Of Palliative Medicine, 11, 3, pp. 459-469, Academic Search Premier, EBSCOhost.
Olver, I, & Eliott, J 2008, ‘The perceptions of do-not-resuscitate policies of dying patients with cancer’, Psycho-Oncology, 17, 4, pp. 347-353, Academic Search Premier, EBSCOhost.
Park, Y, Kim, J, & Kim, K 2011, ‘Changes in how ICU nurses perceive the DNR decision and their nursing activity after implementing it’, Nursing Ethics, 18, 6, pp. 802-813, Academic Search Premier, EBSCOhost.
Perron, N, de Torrente, A, & Morabia, A 2002, ‘Evaluation of do not resuscitate orders (DNR) in a swiss community hospital’, Journal Of Medical Ethics, 28, 6, p. 364, Academic Search Premier, EBSCOhost.
Postovsky, S, Levenzon, A, Ofir, R, & Arush, M 2004, ‘“DO NOT RESUSCITATE” ORDERS AMONG CHILDREN WITH SOLID TUMORS AT THE END OF LIFE’, Pediatric Hematology & Oncology, 21, 7, pp. 661-668, Academic Search Premier, EBSCOhost.
Puri, VK 2006, ‘DNR policies in North America: A procedural morass – resuscitation practices revisited’, Indian Journal Of Critical Care Medicine, 10, 1, pp. 35-39, Academic Search Premier, EBSCOhost.
Silveira, M, Buell, R, & Deyo, R 2003, ‘Prehospital DNR Orders: What Do Physicians in Washington Know?’, Journal Of The American Geriatrics Society, 51, 10, p. 1435, Academic Search Premier, EBSCOhost.
Sulmasy, D, Sood, J, Texiera, K, McAuley, R, McGugins, J, & Ury, W 2006, ‘A Prospective Trial of a New Policy Eliminating Signed Consent for Do Not Resuscitate Orders’, JGIM: Journal Of General Internal Medicine, 21, 12, pp. 1261-1268, Academic Search Premier, EBSCOhost.
Teno, J, Gozalo, P, Mitchell, S, Bynum, J, Dosa, D, & Mor, V 2011, ‘Terminal Hospitalizations of Nursing Home Residents: Does Facility Increasing the Rate of Do Not Resuscitate Orders Reduce Them?’, Journal Of Pain & Symptom Management, 41, 6, pp. 1040-1047, Academic Search Premier, EBSCOhost.
Torke, A, Sachs, G, Helft, P, Petronio, S, Purnell, C, Hui, S, & Callahan, C 2011, ‘Timing of Do-Not-Resuscitate Orders for Hospitalized Older Adults Who Require a Surrogate Decision-Maker’, Journal Of The American Geriatrics Society, 59, 7, pp. 1326-1331, Academic Search Premier, EBSCOhost.
Truog, RD 2010, ‘The Conversation Around CPR/DNR Should Not Be Revived—At Least for Now’, American Journal Of Bioethics, 10, 1, pp. 84-85, Academic Search Premier, EBSCOhost.
Trunk, K, Benkert, B, Quäck, N, Münch, R, Scheer, M, Garbe, J, Jänsch, L, Trost, M, Wehland, J, Buer, J, Jahn, M, Schobert, M, & Jahn, D 2010, ‘Anaerobic adaptation in Pseudomonas aeruginosa: definition of the Anr and Dnr regulons’, Environmental Microbiology, 12, 6, pp. 1719-1733, Academic Search Premier, EBSCOhost.
Weise, KL 2005, ‘The Spectrum of Our Obligations: DNR in Public Schools’, American Journal Of Bioethics, 5, 1, pp. 81-83, Academic Search Premier, EBSCOhost.
Yuanmay, C, Chin-Feng, H, & Chia-Chin, L 2010, ‘Do-not-resuscitate orders for critically ill patients in intensive care’, Nursing Ethics, 17, 4, pp. 445-455, Academic Search Premier, EBSCOhost.
Yuen, J, Reid, M, & Fetters, M 2011, ‘Hospital Do-Not-Resuscitate Orders: Why They Have Failed and How to Fix Them’, JGIM: Journal Of General Internal Medicine, 26, 7, pp. 791-797, Academic Search Premier, EBSCOhost.